First-in-human trial shows promise in treating neuroblastoma
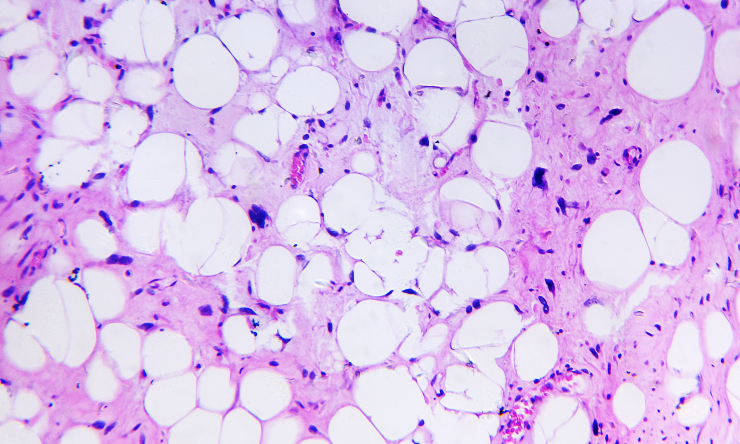
Neuroblastoma is the most common extracranial solid cancer in children, and patients with high-risk disease are challenging to treat. In a promising development, researchers at Baylor College of Medicine released initial findings from the first two patients treated in a Phase 1, first-in-human clinical trial of a new form of immunotherapy to treat neuroblastoma using genetically engineered natural killer T cells (NKTs). The findings were presented today at the annual American Society of Cell & Gene Therapy (ASGCT) Meeting.
Dr. Andras Heczey, assistant professor of pediatrics - hematology and oncology, and Dr. Leonid Metelitsa, professor of pediatrics – oncology, both at Baylor College of Medicine and Texas Children’s Hospital, have studied NKTs and neuroblastoma for years with the goal of making research breakthroughs that lead to new therapies.
“This trial marks the first time highly pure and genetically engineered NKTs are being evaluated in humans to define their safety parameters and measure antitumor activity. For both patients thus far, these infusions have been safe and very well tolerated, further boosting our enthusiasm,” Heczey said.
NKTs are a subgroup of white blood cells that can enter tumor tissues and indirectly suppress tumor growth by attacking tumor-supportive macrophages. GD2 is a molecule that is found on the surface of almost all neuroblastoma cells.
Heczey, Metelitsa and colleagues have genetically engineered NKT cells to express a protein known as the GD2-specific chimeric antigen receptor (GD2-CAR), which enables these immune cells to directly kill neuroblastoma cells by targeting GD2. The GD2-CAR construct also includes a mediator known as interleukin-15, which should enable NKTs to function better in the low-oxygen tumor microenvironment and last longer following infusion into patients.
“GD2-CAR-engineered NKTs recognize GD2 on the cell surface of neuroblastoma cells, which they destroy specifically and effectively in the laboratory setting while maintaining their ability to indirectly attack neuroblastoma by eliminating tumor-associated macrophages,” Heczey said. “There is tremendous promise in this therapy, and this clinical trial is helping to determine how to best implement it for patients.”
The key aims of the clinical trial are to establish the maximum tolerated dose of GD2-CAR NKT cells, evaluate their effect on the tumor, measure how long they can be detected in the patient’s blood, and characterize their effect on the patient’s neuroblastoma.
These aims are being accomplished by generating GD2-CAR NKTs directly from the blood of individual neuroblastoma patients and then re-infusing the engineered cells back into the patient. Toxicities are monitored according to NCI guidelines.
“I’m very excited about reporting the first results of this clinical testing of CAR-redirected NKT cells in children with neuroblastoma,” Metelitsa said. “It took more than 15 years from when we discovered NKT cell presence in tumors and their association with favorable outcomes in neuroblastoma patients, to developing a clinical-grade therapeutic product, which combines natural and engineered anti-tumor properties of NKT cells.”
Of the two patients who have been treated thus far with the therapy, none experienced side effects associated with CAR-NKT cell therapy. One of the patients experienced a stable disease. Another patient experienced a very strong partial response following the first infusion with complete regression of one of two metastatic lesions and nearly complete regression of another. This patient was approved by the FDA for a second infusion.
“Neuroblastoma is a challenging tumor type, and this clinical trial is addressing a significant need in the treatment of pediatric solid tumors,” Heczey said. “Our goal is to find a safe option to effectively treat high-risk neuroblastoma, and this clinical trial has presented us with a promising option. We will continue to monitor and follow these patients.”
The results of this study help inform clinical development of NKT cell-based immunotherapy for neuroblastoma and have broad applicability to other types of cancer in the future. Heczey and Metelitsa also hope this research will help advance the development of an off-the-shelf approach, allowing patients to be treated more universally, a topic Metelitsa explored in two additional presentations at the meeting.
Voluntary enrollment in the GINAKIT2 gene transfer research study using these special immune cells remains open to patients whose neuroblastoma has either come back after treatment or has not responded to the standard, existing therapies and medicines used to treat it. Cell Medica has licensed CAR-NKT cell technology and supports further preclinical and clinical development of this therapy through its collaboration with Baylor.
Metelitsa also conducted an educational session about harnessing the natural and engineered properties of iNKT cells for adoptive cancer immunotherapy.
Heczey and Metelitsa also are members of the Dan L Duncan Comprehensive Cancer Center at Baylor College of Medicine. This study is supported by Alex’s Lemonade Stand Foundation. Learn more information about GINAKIT2, and how to enroll.