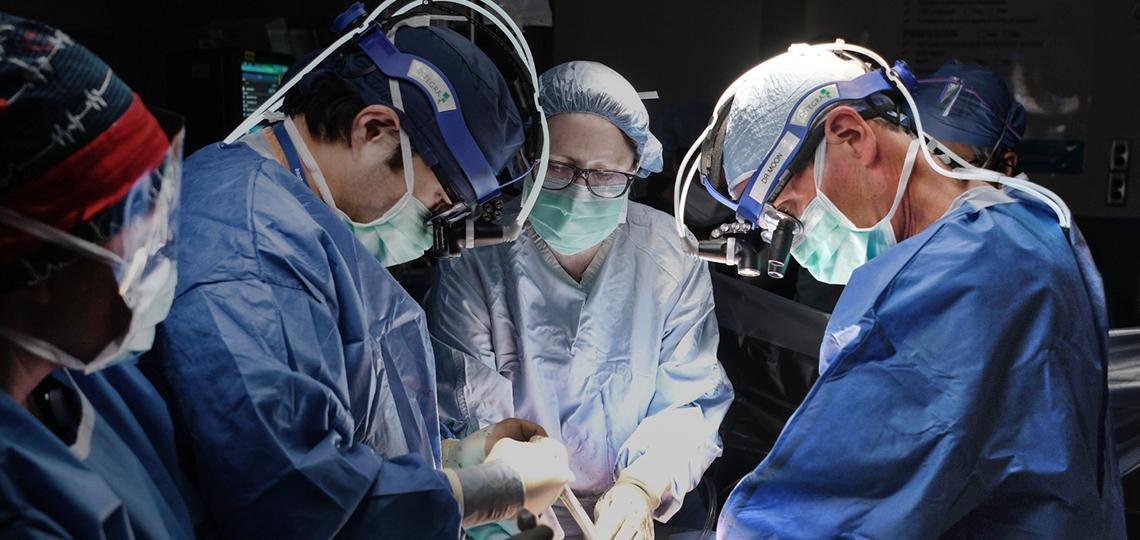
Division Highlights
- The Cardiothoracic Surgery team has performed more than 7,500 repairs of the aorta and over 3,800 repairs of thoracoabdominal aortic aneurysms, representing one of the largest experiences in aortic surgery the world
- Our surgeons at Baylor St. Luke’s have performed more than 1,000 transcatheter aortic valve replacement procedures and participate in multiple mitral and tricuspid valve clinical trials
- Consistently ranked in the Top 20 for heart surgery by U.S. News & World Report, with special distinction in heart bypass surgery, aortic valve surgery and abdominal aortic aneurysm repair at Baylor St. Luke’s
- Our heart surgery program at the Michael E. DeBakey VA Medical Center is one of the busiest VA cardiac centers in the United States, and is one of only three VA centers in the United States performing on-site heart transplantation

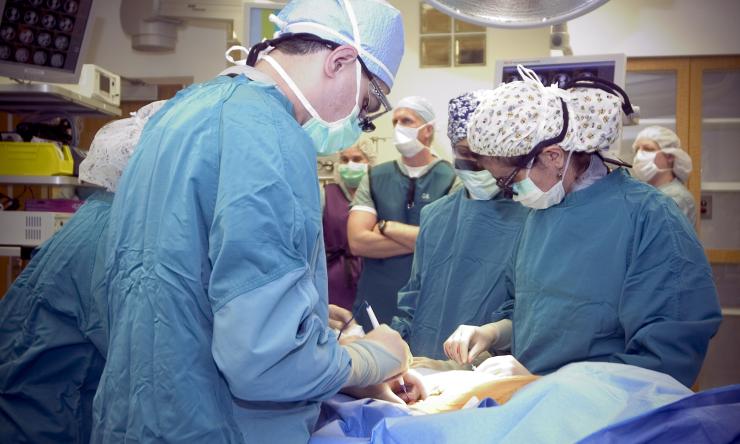
Education
The Division of Cardiothoracic Surgery offers training in thoracic and aortic surgery and a T32 Research Training Program.
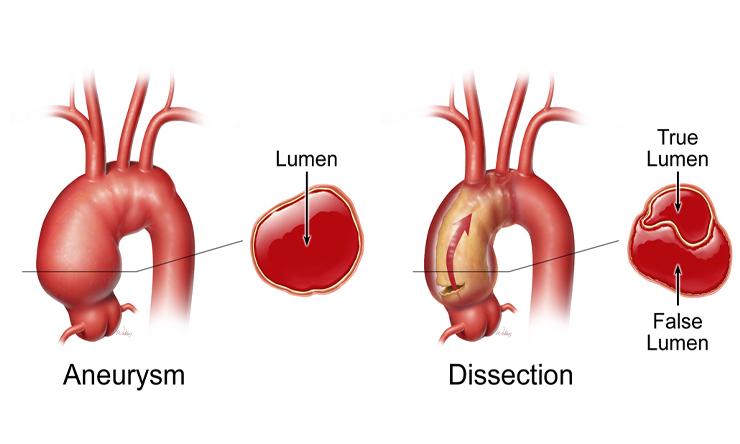
Research
Explore clinical and basic science research from the Cardiothoracic Surgery Division.