The Division of Surgical Oncology is an integral component of the multidisciplinary teams at the Dan L Duncan Comprehensive Cancer Center (DLDCCC). Funded by NIH, the DLDCCC focuses on research-driven patient care across various scientific disciplines. Our scientists and clinicians collaborate closely with patients to treat cancers such as pancreatic, liver, breast, and endocrine cancers.
Surgical Oncology Research Programs
The Surgical Translational Oncology Laboratory , led by Dr. E. Ramsay Camp, focuses on understanding mechanisms responsible for chemotherapy and radiation resistance in pancreatic and colorectal cancer. The research is supported by a VA Merit Award and an industry award from Merck, which supports the investigation into a novel chemo-immunotherapy strategy for pancreatic cancer.
The Virus-Like Particle Translational Oncology Lab, led by Dr. Qizhi Cathy Yao and her team, is dedicated to understanding the molecular mechanisms of pancreatic cancer tumorigenesis. They are developing novel immunotherapeutic approaches to cancer treatment, supported by funding from the NIH, CPRIT, and the VA. The team has also developed 25 lines of patient-derived xenografts, fully characterized with mutation and gene expression data, for future research projects.
An NIH-sponsored consortium studying pancreatic cancer, led by Dr. William E. Fisher, has established a comprehensive tissue repository that supports pancreatic research at Baylor College of Medicine and is shared with researchers nationwide.
Basic Science and Translational Labs led by Dr. Changyi Johnny Chen actively investigates the effects and the molecular mechanisms of several cardiovascular risk factors on biochemical pathways associated with endothelial cell functions. Their comprehensive studies also analyze human cancer specimens, clinical outcomes, established cell lines, a nude mouse model, and a genetically engineered mouse model of pancreatic cancer called the KPC model.
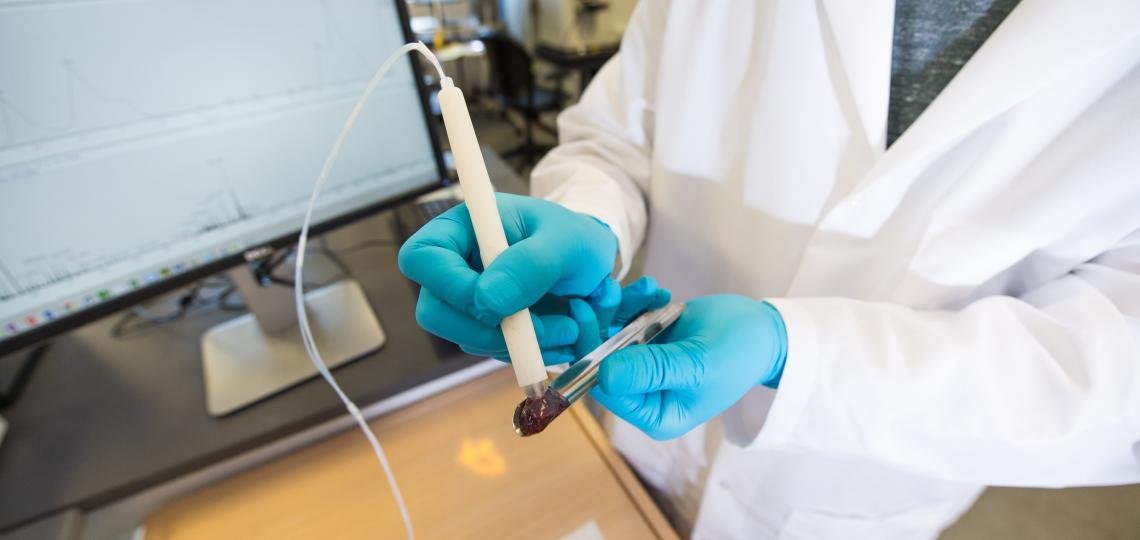
Direct mass spectrometry for tissue analysis and disease detection, pioneered in the Eberlin Lab for Medical Mass Spectrometry, aims to identify metabolic markers of cancer and other diseases. They are also working on the development of mass spectrometry technologies and medical devices for surgical use.
Innovations in Breast Cancer Treatment, led by Dr. Alastair Thompson, challenges aggressive treatment strategies for ductal carcinoma in situ (DCIS), which accounts for up to 25% of diagnosed breast cancer cases. Recent studies suggest that active surveillance may be just as safe as traditional treatments, which often cause physical, emotional, and financial harm.
The Michael E. DeBakey Center for Nano-Biophotonics is led by Director, Dr. Thomas Milner who is funded by a Cancer Prevention and Research Institute of Texas (CPRIT) award. Dr. Milner oversees the translation of nano-biophotonic technologies into clinical applications for cancer diagnostics and therapy and fosters collaborations with clinicians, scientists, and engineers within Baylor, the Texas Medical Center, and across Texas. Together, they design, develop, and demonstrate novel photonic devices aimed at improving human health and well-being.
At the interface of medicine, bioengineering, chemistry and pharmaceutics, Drs. Ghanashyam Archarya and Crystal Shin are leading the mission in developing broadly applicable drug delivery systems and biomaterials for surgical applications with enhanced therapeutic efficacy through the integration of nanotechnology and 3D bioprinting technology.