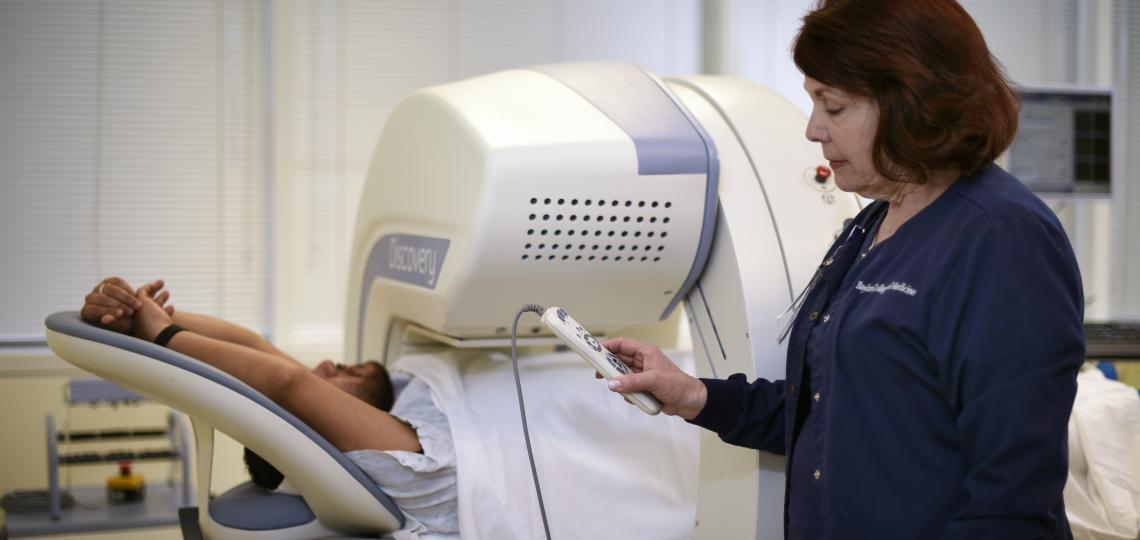
Our comprehensive, integrated, patient-centered approach to the prevention, care, and treatment of cardiovascular diseases is further improved through the close proximity of specialties and shared technology within Baylor Medicine and our affiliated institutions. Our treatment begins with state-of-the-art testing to ensure top-quality patient care.
Non-Invasive Tests
The electrocardiogram (ECG; sometimes abbreviated EKG) is a non-invasive test that records the electrical activity generated by the heart. This electrical activity is recorded from the patient's body surface (limbs and chest) by 10 electrodes held snugly against the skin by elastic bands or suction cups. The test takes 5-10 minutes to complete and yields information about the heart rhythm and rate, hypertrophy (thickness of the heart muscle) and chamber enlargement, presence of an old or ongoing heart attack (myocardial infarction), or evidence of impaired blood supply (ischemia). This is one of the most informative tests performed upon the heart.
A stress test is a non-invasive test that gives important information about the exercise capacity and the presence or absence of blockages or narrowing in the coronary arteries (or blood vessels that supply blood to the heart). The "stress" portion of the test can be performed on a treadmill, or by injection of a medication. This test provides information about the presence underlying heart disease and how it has affected your general health.
Also referred to as an "echo," an echocardiogram is a non-invasive ultrasound test that uses sound waves emitted from a probe that is pressed against your chest wall or one that is swallowed to get a better view of the heart from the esophagus. The echoes or sound waves that bounce back from the emitted sound waves permit your doctors to see how your heart, heart valves, and large blood vessels look and function.
Electrophysiologists order an echo primarily to see if there is an underlying problem in any of the above structures that could explain, cause or complicate a rhythm disorder. An echo performed from your esophagus is very important in looking for blood clots if you have atrial fibrillation or atrial flutter and a cardioversion and/or radiofrequency ablation procedure is planned. If cardioversion is performed with blood clots present, there is a much greater risk of suffering a stroke.
The Signal-Averaged Electrocardiogram (SAECG) is a non-invasive test that records the heart's electrical activity. It is like the electrocardiogram but uses specialized computer processing to magnify the heart muscle's signal (QRS) and search for abnormal electrical activities called late-potentials. These are not seen on the regular ECG. The presence of late-potentials helps identify individuals at risk for developing life-threatening arrhythmias, such as ventricular tachycardia or ventricular fibrillation. This test takes 30 to 40 minutes to perform. There are no restrictions on food, liquids, or medications before this test.
A T-wave alternans test is another type of non-invasive test that measures the heart's electrical activity. It is a special type of ECG that requires additional accompanying computer processing to detect small changes in the heart's electrical activity that occur on a beat-to-beat basis. These changes are not readily seen on the regular ECG. The test specifically looks at the size of the T-wave.
The presence of alternating sizes of T-waves (or T-wave alternans) is abnormal and identifies individuals at a higher risk of life-threatening arrhythmias such as ventricular tachycardia and fibrillation. A T-wave alternans test is usually done in conjunction with a stress test with the exception that some extra monitoring electrodes may be required. The preparation is the same as for the stress test.
Arrhythmias that are not documented on the routine electrocardiogram (ECG) will usually require some type of home (ambulatory) documentation. The Holter monitor is a small compact magnetic tape electrocardiographic recorder. Electrodes are placed firmly on the skin of the chest beneath the patient's clothing and an ECG record of 12-24 hours is obtained. The recorder is returned the following day and the total ECG record is retrieved from the magnetic tape and interpreted by the physician. This technology is helpful in the diagnosis of paroxysmal (intermittent) rhythm disturbances and essential for selecting proper treatment and at times for evaluating the subsequent outcome on treatment.
There are many circumstances wherein a rhythm disturbance, or symptoms presumed to be due to a rhythm disturbance, occur infrequently and cannot be documented during a single 24-hour or 48-hour record, such as that obtained with a Holter monitor. These infrequent events require that electrocardiographic documentation be recorded at the time of the symptoms. An electrocardiographic event monitor is loaned to such patients for periods from one and up to three months with instructions regarding its simple application to the chest wall at the time of symptoms. The electrocardiogram that is recorded is transmitted over the telephone to a central station, from which it is transferred to your physician for interpretation.
A head upright tilt test (HUTT) is usually performed as part of the evaluation for syncope (passing out). It specifically screens for one of the more common causes of fainting called neurocardiogenic syncope. Individuals who suffer from this disorder usually pass out after being in the standing or sitting position for prolonged periods of time, although in some individuals the duration can certainly be brief). During a tilt test, the objective is to provoke one of these spells by placing the patient in an upright position while constantly monitoring blood pressure and heart rate.
Preparation for the test:
- Nothing to eat or drink overnight or at least six hours prior to the test.
- Make sure to ask your physician about taking your medications, particularly if you are diabetic and are on insulin.
- Wear comfortable clothes and shoes.
Procedure
You will be placed on a flat comfortable table. A nurse will place electrodes on your chest and a blood pressure cuff on your wrist and/or arm to monitor your heart rate (HR) and blood pressure (BP) continuously throughout the procedure. A recording of your blood
pressure and heart rate will be done at baseline in the lying position, after which the table will be brought upright or tilted to a 70-degree inclination. Blood pressure and heart rate are then monitored continuously and values are recorded every 3 minutes. Unless the test is positive (your BP and/or HR fall and you faint or experience a near-faint), you will remain at 70-degrees for 30 minutes. At 30 minutes, additional maneuvers will be done to try to provoke an abnormal test.
The first of these is massaging your upper neck on both the left and right sides (called carotid massage) and the second is giving a small dose of nitroglycerin under the tongue. After nitroglycerin is given, the tilt is continued for another 10-15 minutes. The test is terminated if you have a positive test or did not respond to any of the above.
After the test:
- You will be observed for 10-15 minutes.
- You can eat.
- You can go home on the same day.
A cardiac MRI is a non-invasive test that uses magnetic waves and the differing magnetic properties of our bodies to obtain high-resolution pictures of the heart and surrounding structures. It also permits the assessment of heart valves and overall heart function. Electrophysiologists use cardiac MRIs generally to evaluate for the presence of underlying heart disease.
More specific uses include evaluating the right ventricle (the right pumping chamber) when an arrhythmia is suspected of arising from there (the right ventricle is difficult to evaluate using other techniques), and ascertaining the origin and course of the coronary arteries when there is suspicion that this is abnormal.
Certain individuals are born with abnormally coursing arteries that predispose them to arrhythmias. The test usually takes 45 minutes to an hour to perform.
Invasive Tests
Cardiac catheterization involves the insertion of a long, thin tube into a blood vessel in your groin or arm. The tube will be gently directed to the heart and to the origin of the coronary arteries, as well as into the left ventricle, the heart's main pumping chamber. Dye is then injected into the coronary artery while x-ray pictures are taken. Pictures can also be taken of the left ventricle. Pressures on the left side of the heart are simultaneously measured and recorded.
A cardiac catheterization permits confirmation for the presence or absence of significant blockages in the coronary arteries can show evidence for previous, recent, or ongoing heart attacks can evaluate valve function and overall heart muscle performance.
These are important information for the electrophysiologist in determining probable causes for arrhythmias as well as help in tailoring the best treatment to suit an individual patient's needs. In many instances the arrhythmia is caused by a blockage; this can be treated at the same time with angioplasty.
An implantable loop recorder is a small device about the size of an average-sized man's thumb that is placed under the skin to diagnose causes of syncope (or passing out) or recurrent palpitations (heart pounding) that have remained elusive or could not be diagnosed after monitoring with a Holter and external loop recorder and/or even after an EP test.
The way this device works is that it constantly monitors the heart rhythm and if one experiences any symptoms or passes out, the device can be activated to record the heart rhythm at the time of activation as well as several minutes before and after activation. That way, a detailed view of the heart's rhythm is available for analysis. Activation can be done using an external activator device or it can also be done automatically.
How do I prepare for the Implantable Loop Recorder?
- Nothing to eat or drink overnight or at least six hours before the procedure.
- Remember to ask your physician for instructions about taking your scheduled medications especially if you are diabetic (on insulin or pills) and/or are taking pills that can make you prone to bleeding (i.e. Coumadin or warfarin, Plavix or clopidogrel).
- An intravenous (IV) line may be inserted prior to the procedure.
- An antibiotic may be given through the IV line to reduce the risk of infection.
What occurs during the Implantable Loop Procedure?
laboratory or operating suite. Before anything is done, an area of your chest is selected that yields the best signal from your heart; this is usually on the left mid-upper chest. The selected area is then shaved (if applicable), cleaned with antiseptic, and covered with a sterile drape. This is then numbed with a local anesthetic so that a small incision approximately two cm. can be made to insert the device. This incision will be closed with a few stitches or staples. No x-rays will be used during the procedure. You will be sedated according to what your physician deems is necessary.
What occurs after the Implantable Loop Procedure?
- You will be instructed on how to operate the device.
- You may be given a short course of antibiotics.
- You most likely will be sent home on the same day.
- You will be instructed on wound care. You may get the wound wet after five days.
- After 10-14 days. An office visit will be scheduled to check the wound and remove stitches.
An electrophysiology study or EPS is an invasive test that examines the electrical properties of the heart by the placement of special catheters inserted via the leg, arm, or neck. An EP study enables your physician to search for explanations for symptoms such as palpitations, irregular heartbeats, fainting, and near-fainting spells. It also helps your doctor decide on the best course of treatment (medicines, a pacemaker, defibrillator, RF ablation, or surgery) which can be done in conjunction with the EP study or scheduled at a later date.
How to prepare for the Electrophysiology Study procedure?
- Nothing to eat or drink overnight or at least six hours before the procedure.
- Remember to ask your physician for instructions about taking your scheduled medications especially if you are diabetic (on insulin or pills) and/or are taking pills that can make you prone to bleeding (i.e. Coumadin or warfarin, Plavix, or clopidogrel).
- Your doctor may advise you to stop taking certain medications before your EP study to ensure more accurate results.
- A chest x-ray, electrocardiogram (ECG), and blood work may be obtained. A urine pregnancy test is routinely obtained for all women of childbearing age.
- Get a good night’s sleep.
- An intravenous (IV) line will be inserted through which fluids and medicines can be given.
What occurs during the Electrophysiology Study procedure?
The procedure is usually a same-day admission. The EP lab is similar to the laboratory used for heart catheterizations. During the EPS procedure, you will be awake, but you may be given medications to help you relax. Electrodes will monitor your heart rhythm and rate. This may require that some areas be shaved in preparation.
You will be placed on a flat, cushioned table. The groin area is shaved, sterilized, and numbed so a sheath can be inserted. Through this sheath, temporary pacemaker catheters – about as thick as a piece of spaghetti – are placed in strategic areas of the heart. These catheters record electrical activity inside the heart and allow the physician to artificially "pace" or stimulate your heart. An x-ray machine in the shape of a large C will be placed directly over your body and maneuvered at various angles to allow your physician to watch the catheters and see that they are properly placed. You will receive only intermittent low doses of x-rays.
Your physician will then artificially create different heart rates and will watch for arrhythmias. He may also give some drugs that make your heart rate speed up in an attempt to induce or provoke arrhythmias. During the test, you may experience no symptoms whatsoever, or you may feel a rapid heart rate, skipped beats, light-headedness, chest pain, or discomfort. If you experience any of these problems, please let the physician know. Sometimes you may pass out briefly during the test or an abnormal rhythm may be induced, and it may become necessary to give your heart a mild electric shock to restore your normal rhythm. When you wake up, do not be alarmed if you find an oxygen mask covering your mouth and nose.
If no arrhythmia is found, the catheters are removed, the test is concluded, and you will be returned to your room. If your physician is successful in reproducing your arrhythmia, he may proceed with radiofrequency ablation or placement of a pacemaker or defibrillator.
If the decision is to proceed with radiofrequency ablation, your physician will then make a "map" of your arrhythmia. This electrical map tells your physician where the arrhythmia is coming from, what areas of the heart are necessary to keep the arrhythmia going, and more importantly, it tells your physician where to apply radiofrequency currents to get rid of your arrhythmia. EP studies usually last from two to four hours.
What occurs after the Electrophysiology Study procedure?
- After the catheters are removed, pressure will be applied to the puncture site just enough to stop the bleeding. No stitches are required but a sterile dressing will be applied and can be removed the next day.
- Remain in bed with your leg straight for anywhere between three to six hours. Nurses will assist you when it is OK to get up.
- Keep your head on the pillow.
- Inform the nurse if you have any warmth, pain, or swelling where the catheters were removed.
- If you need to cough, sneeze or strain, hold the dressing down firmly before doing so.
- You will be permitted to eat and drink.
- Your vital signs and catheter insertion site will be checked frequently.
The exact length of your hospital stay is determined by your diagnosis and the treatment option prescribed by your physician. With a regular, uncomplicated EP study, you can usually go home later the same day. If the procedure was long and complicated, or if a pacemaker or defibrillator was implanted, this usually requires an overnight stay.
When the bandages are removed from the catheter insertion site, you may notice a small bruise no larger than a quarter. You may also feel a small lump there. The bruise may become slightly larger and/or darker after you return home. Both of these are part of the body's natural healing process and should disappear completely within two weeks. If you notice a discharge, or feel feverish or become very uncomfortable, please call our office immediately.
Some patients may require no further treatment. Others may require any one of the treatment alternatives described below. Your physician will explain his/her findings and recommendations following your study. However, don't be afraid to ask questions at any time before, during, or after the procedure.