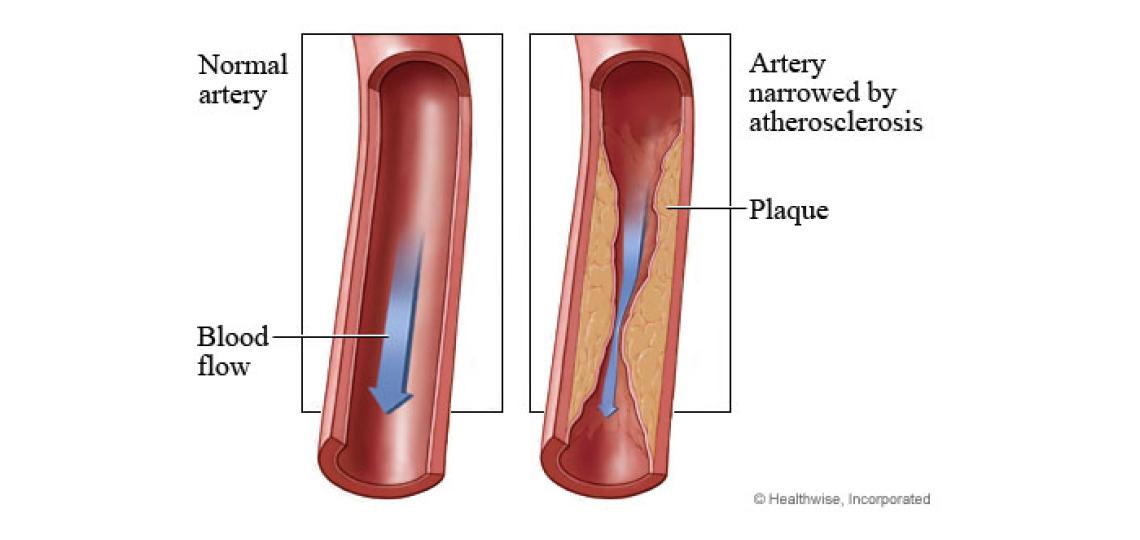
What Is Peripheral Artery Disease?
Lower extremity peripheral artery disease is a condition that develops when the arteries in the legs and feet become narrowed, or occluded, by an accumulation of a fatty substance called plaque, which builds up on the inside walls of the arteries. This narrowing is also called stenosis. As the arteries narrow, blood supply to the muscles and tissues in the legs and feet decreases, causing pain, poor healing, and in severe cases tissue death. Lower extremity artery disease is one manifestation of atherosclerosis, the hardening and narrowing of the arteries due to plaque build-up. Atherosclerosis affects as many as 35 percent of Americans. People with lower extremity artery disease often have other cardiovascular problems causes by atherosclerosis such as carotid artery disease and heart disease.
Dr. Gilani explains peripheral artery disease.
What Are the Risk Factors and Symptoms for Peripheral Artery Disease?
Risk factors for lower extremity artery disease include smoking, which is the most common risk factor for all cardiovascular diseases. Other risk factors include a family history of atherosclerosis, high blood pressure, diabetes, abnormal cholesterol levels, advanced age, and a sedentary lifestyle.
The symptoms of lower extremity artery disease include:
- Claudication, cramping pains while walking, usually in the calf muscles but sometimes in the thighs. Claudication is the most common symptom of this condition.
- Pain in the feet and, as the disease progresses, in the toes while at rest.
- Coolness, numbness, or weakness of the legs and feet.
- Poor healing of wounds in the legs and feet.
- Ulcers of the feet and legs, which develop when the blood supply to tissue is cut off, and which can become gangrenous if untreated.
- Black discoloration of the toes or skin around the occluded artery.
To determine the severity of blood flow impairment to the leg, doctors compare the blood pressure in the ankle to that in arm using a test called the ankle brachial index (ABI).
Doctors may also use imaging tests such as angiography or magnetic resonance imaging (MRI) to determine the location and the extent of the arterial stenosis in the legs.
What Are the Treatments for Peripheral Artery Disease?
Patients whose symptoms are mild to moderate can often manage their disease by making lifestyle changes such as quitting smoking, getting regular exercise – which can be a tremendous help in relieving symptoms – and working with their doctors to take care of related conditions such as diabetes, high blood pressure, and high cholesterol. Doctors may also prescribe blood-thinning drugs or other medications.
Doctors often use minimally invasive procedures such as balloon angioplasty and stenting to relieve the narrowing and improve blood supply to the extremities. These techniques work best when the diseased portion of the artery is relatively small, and when it is easily accessible with a catheter, a very thin tube tipped with surgical equipment that can be inserted into and threaded through a blood vessel. Angioplasty and stenting are often initially very effective in relieving the blockage, but in 30 to 40 percent of patients, the blockage comes back within the first year or two. This re-blocking of the artery is called "restenosis."
An angiogram is a diagnostic imaging test that allows doctors to view blood vessels throughout the body and diagnose blockages, enlargements, clots, and malformations. An angiogram to study the arteries is called an arteriogram; one to study the veins is called a venogram. Before the test doctors inject a dye into the vessels to be imaged using a long, flexible, hollow tube called a catheter, which is usually introduced into the body through a needle puncture in the groin. The dye makes the blood vessels clearly visible on an x-ray image. Your doctor can combine an angiogram procedure with one of the minimally invasive procedures outlined below, which include balloon angioplasty, stenting, atherectomy, cryoplasty, or laser treatment.
During angioplasty, a deflated balloon-tipped catheter is inserted through an artery in the groin and guided to the narrowed segment of the artery. When the catheter reaches the blockage the balloon is inflated, compressing the plaque and widening the artery.
In some cases, doctors may place a stent, a small mesh support tube, at the site of the blockage during angioplasty. The stent is collapsed when it is placed on the tip of the catheter and inserted into the body. Once the catheter reaches the blockage, surgeons expand the stent by inflating the balloon. The stent is left permanently in the artery to provide a reinforced channel through which blood can flow. Some stents (drug-eluting stents) are coated with medication that helps prevent the formation of scar tissue.
During atherectomy doctors use a specially equipped catheter to remove plaque from an artery's lining. Performed in conjunction with angioplasty, the catheter and atherectomy device is inserted into the body through a tiny puncture site and is advanced through the artery to the site of the blockage where the device is activated. Atherectomy devices are equipped with a rotating blade, which shaves plaque off of the inside of the artery walls; or a burr, which grinds hardened plaque from the artery wall. The removed plaque is then suctioned into the catheter and removed from the body.
During cryoplasty doctors both freeze and dilate the artery wall with a balloon. This freezing action causes the plaque to break apart in tiny, uniform pieces and is thought to help prevent the smooth muscle cells in the artery wall from secreting a substance that promotes restenosis.
Doctors perform laser angioplasty using a catheter tipped with a laser. When the laser is in position, it emits pulsating beams of light that vaporize the plaque.
In situations where artery disease is severe, your doctor may recommend a leg bypass procedure in which a new blood vessel is reconstructed in the leg to provide better blood flow to heal leg wounds or relieve leg pain.