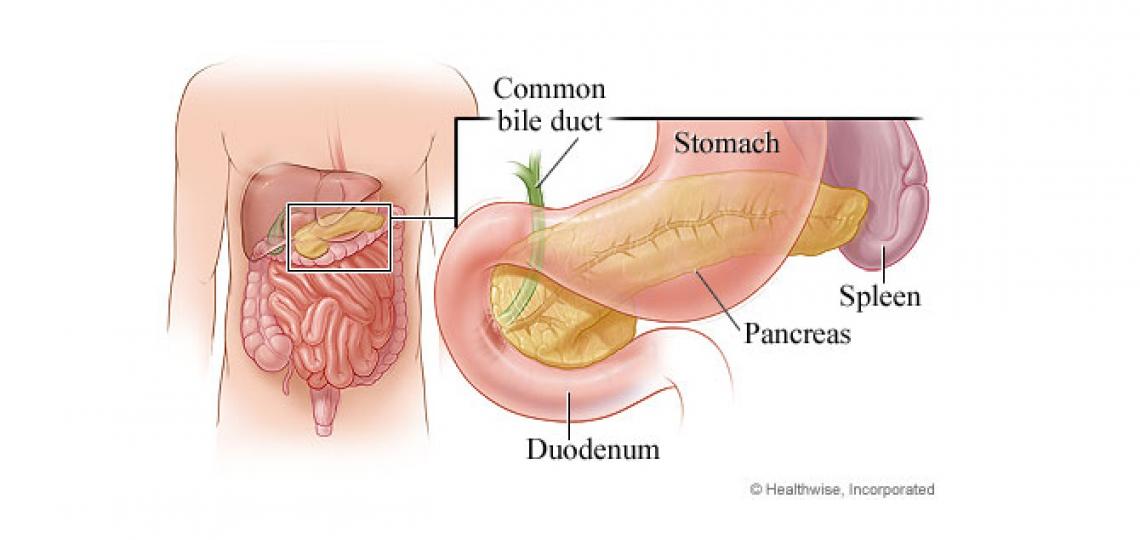
There are no established guidelines for the screening of pancreatic cancer. However, those at high-risk for pancreatic cancer, due to genetic predisposition, may benefit from pancreatic cancer screening. A series of tests and procedures may be done during a patient’s evaluation.
High-risk individuals with a genetic predisposition for pancreatic cancer, patients who have been diagnosed with chronic pancreatitis, and patients over the age of 50 with new onset diabetes should be screened.
Tests
Some of the tests used to screen for pancreas cancer are:
- MRI (Magnetic Resonance Imaging)
- EUS (Endoscopic Ultrasound)
- ERCP (Endoscopic Retrograde Cholangiopancreatography)
- CT Scan (Computed Tomography)
- Laparoscopy and biopsies
- Checking your blood for tumor markers
What to Expect
A pancreatic cancer workup at the Elkins Pancreas Center includes the following:
- A clinic visit with a pancreas specialist who will assess risk factors of pancreatic cancer such as smoking, obesity, presence of chronic pancreatitis or exocrine pancreatic insufficiency or new onset diabetes.
- MRI screening of the pancreas
- Endoscopic Ultrasound with possible Fine Needle Aspiration of any discovered lesion
- A CA 19-9 tumor marker blood test
- Genetic counseling for patients with familial pancreatic cancer or patient with single first degree relative with pancreatic cancer under the age of fifty
- A multidisciplinary tumor board will be assigned your individual case, discussing any concerning lesions discovered during the screening
Tumor Board
A tumor board consists of physicians from multiple disciplines such as surgery, oncology, gastroenterology, radiation oncology, radiology and pathology that will discuss your case as a team and come up with an individual treatment plan for you.
If work-up is negative, the above work-up will be repeated in two to three-year intervals.
© 2016-2019 Healthwise, Incorporated.








 Credit
Credit