What Is the Connection Between Diabetes and Limb Loss?
Diabetes is a multifaceted condition that can result in severe complications, including limb loss. Two major concerns are poor circulation and diminished sensation in the feet, which heighten the risk of foot ulcers, non-healing wounds, and infections. Without proper treatment, these issues can worsen and ultimately lead to limb amputation. Understanding the risk factors is crucial to prevention and early intervention.
Individuals at higher risk include:
- Long-standing diabetes or kidney failure: Chronic conditions that compromise circulation and healing.
- Current or former heavy smokers: Smoking damages blood vessels, significantly impairing circulation and wound healing.
- People with non-healing foot wounds: These can be early indicators of poor circulation or infection.
- Adults over age 55: Age-related vascular changes can increase the likelihood of complications.
- Those with claudication (leg pain during exercise): Progressive pain in the calves while walking or running may signal poor blood flow and vascular disease.
Recognizing these risk factors and seeking prompt medical attention can make the difference in preserving limb function and quality of life.
Jose Samano faced a dire situation with a severe foot infection and peripheral vascular disease which led multiple surgeons to suggest leg amputation. However, Dr. Tyler Coye, a foot surgeon at Baylor Medicine specializing in limb salvage, saw the potential to save Samano's leg.
Can Amputation Be Prevented?
STEP: Save the Extremity Program
Save the Extremity Program (STEP), part of the Division of Vascular Surgery and Endovascular Therapy, is a clinical and research collaboration dedicated to recognizing diabetic foot-related conditions and providing interventional treatments to prevent amputations and save limbs. Our exceptional STEP team includes vascular surgeons, podiatrists, wound care specialists and researchers, who give patients access to the latest, state-of-the-art, minimally invasive vascular interventions, open surgery, wound care and wearable technology available. Our STEP professionals work to keep patients complication free, mobile and independent. Call for more information today at (713) 798-5700.
What Is the "Toe and Flow" Model?
Our limb salvage program seamlessly integrates vascular surgery and podiatry for both the outpatient and inpatient.
Our limb salvage program is built on the toe and flow model, a seamless integration of podiatry and vascular surgery for comprehensive care of both outpatients and inpatients.
Podiatrists are often the first to identify signs of peripheral artery disease (PAD), a critical factor in limb preservation. In our program, podiatrists collaborate closely with vascular surgeons and radiologists to diagnose and treat conditions affecting the foot, ankle, and lower extremity.
- Flow refers to the vital role of blood flow in wound healing. Vascular surgeons are experts in restoring and optimizing circulation, ensuring the foundation for recovery.
- Toe encompasses all procedures and care necessary to heal the foot and toes. Podiatrists bring specialized expertise in foot surgery, wound management and limb preservation.
Together, this integrated approach ensures the best outcomes for patients facing complex foot and vascular conditions.
How Is Diabetic Foot Diagnosed and Treated?
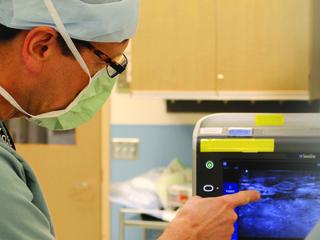
Diagnosing and treating diabetic foot conditions requires a multidisciplinary approach, combining advanced diagnostic tools and specialized care from both vascular surgeons and podiatrists to ensure optimal outcomes.
Diagnosis
Our team employs state-of-the-art diagnostic tools to evaluate arterial health and foot integrity.
- Vascular Diagnostic Tools:
- Ultrasound-guided imaging: Provides real-time visualization of arterial flow, identifying blockages with precision.
- Advanced imaging techniques: Tools like CT angiography and MRI provide detailed evaluations of blood vessel health and tissue structures, guiding targeted interventions.
- Podiatric Diagnostic Tools:
- Monofilament testing: Detects loss of protective sensation in the feet, a critical early sign of neuropathy.
- Biomechanical assessments: Evaluates gait, pressure points, and structural abnormalities that increase the risk of ulcers.
- Wound evaluation: Employs advanced techniques, including tissue perfusion analysis to assess wound oxygenation and viability.
Vascular Procedures
Our highly trained group of surgeons have mastered the following procedures that lead to increase in the blood flow to the foot, which then allows better healing rates.
Deep vein arterialization (DVA) is a minimally invasive procedure used for patients with chronic limb-threatening ischemia (CLTI) who have no remaining surgical or endovascular options. This technique reroutes blood from an artery directly into a deep vein, bypassing blocked vessels to restore circulation in the lower limb. The procedure involves inserting a catheter into a major artery, crossing the blockage using a guidewire and creating a new connection between the artery and vein using a stent. Drug-coated balloons or additional stents may be used to keep the pathway open and optimize blood flow. By improving oxygenation in the foot, DVA may reduce pain, promote wound healing and help prevent amputation in patients with otherwise un-reconstructable vascular disease.
Angioplasty and stent placement is a common procedure to restore blood flow in narrowed or blocked arteries. During the procedure, a catheter with a small balloon at its tip is guided to the affected artery and inflated to widen the vessel. In many cases, a stent—a small mesh tube—is placed to keep the artery open and prevent it from collapsing. Stents may be bare metal or drug-coated to reduce the risk of re-narrowing (restenosis). This procedure is widely used to treat conditions like peripheral artery disease (PAD) and coronary artery disease, helping to improve circulation, wound-healing, and mobility while reducing pain.
Atherectomy is a minimally invasive procedure used to remove plaque buildup from the walls of arteries, improving blood flow in patients with peripheral artery disease (PAD). Unlike angioplasty, which compresses plaque against the artery walls, atherectomy physically removes the blockage using a catheter equipped with a rotating blade, laser or orbital mechanism. This technique is particularly beneficial for heavily calcified plaques or lesions in areas that are difficult to treat with angioplasty alone. Atherectomy can be performed as a standalone procedure or in combination with angioplasty and stenting to enhance long.
Drug-coated balloon angioplasty and stenting is a specialized procedure that helps restore blood flow in narrowed arteries while reducing the risk of re-narrowing. Similar to traditional angioplasty, a catheter with a balloon at its tip is guided to the blockage and inflated to widen the artery. However, in this procedure, the balloon is coated with antiproliferative medication that is released into the artery wall, helping to prevent restenosis. A stent may also be placed to provide structural support and keep the vessel open. This approach is commonly used in the treatment of PAD, offering improved long-term results compared to standard angioplasty alone.
Retrograde transpedal endovascular therapy is an advanced technique used to restore blood flow in patients with complex arterial blockages, particularly in the lower limbs. Unlike traditional endovascular procedures that access the artery from above, this technique approaches the blockage from below, using small arteries in the foot (pedal arteries) to reach the affected area. A catheter is inserted through a tiny incision in the foot, and a guidewire is used to navigate past the blockage. Angioplasty, stenting or atherectomy may then be performed to clear the artery and improve circulation. This method is particularly useful for patients with chronic total occlusions (CTOs) that cannot be treated with conventional approaches.
Open bypass surgery is a traditional surgical procedure used to reroute blood flow around a blocked or severely narrowed artery. In this procedure, a healthy vein or synthetic graft is used to create a new pathway for blood to bypass the diseased section of the artery. The graft is sewn into place above and below the blockage, allowing blood to flow freely to the lower limb. Open bypass is often recommended for patients with severe peripheral artery disease (PAD) or chronic limb-threatening ischemia (CLTI) when minimally invasive treatments like angioplasty or stenting are not viable. Although it requires a longer recovery time than endovascular procedures, bypass surgery provides durable, long-term results for restoring circulation and preventing limb loss.
Podiatric Procedures
- Surgical Debridement
- Tendon Lengthening Procedures
- Partial Foot Amputations
- Advanced Skin Substitutes
- Negative Pressure Wound Therapy (NPWT)
- Rotational, Advancement, and Transposition Flaps
- Bone Resection Procedures
- Custom Orthotics and Offloading Devices
- Pedal Soft Tissue Coverage Techniques
- Infection Control Procedures
This comprehensive approach combines advanced surgical techniques, cutting-edge technology, and a multidisciplinary strategy to maximize patient outcomes in diabetic limb salvage.
What to Expect From Your Visit
The primary goal in ulcer management is to heal the wound as quickly as possible. Prompt intervention minimizes the risk of infection, hospitalization and potential amputation.
During your visit with a wound specialist, several essential steps may be taken to effectively manage your foot wound:
- Assessment of blood flow: Ensuring proper circulation is critical for healing and preventing complications.
- Wound debridement: Removal of dead or infected tissue to promote healthy tissue growth.
- Application of medications or dressings: Specialized treatments and dressings will be applied to protect the wound and support healing.
- Infection prevention: Antibiotics may be prescribed to reduce the risk of infection or address existing concerns.
- Offloading: Reducing pressure on the affected area is vital for healing. This may involve the use of a custom shoe, boot or other offloading devices.
Your specialist will create a personalized treatment plan designed to optimize wound healing and prevent further complications.
Will I Require Surgery?
Most non-infected foot wounds can be treated successfully without surgery. However, if conservative treatments do not achieve the desired results, surgical intervention may be necessary. Depending on your condition, surgical options may include:
- Bone removal or shaving: Addressing structural issues or reducing pressure points to facilitate healing.
- Surgical wound debridement: Cleaning the wound to remove dead tissue and reduce the risk of infection.
- Correction of foot deformities: Procedures to address issues such as hammertoes, bunions or bony prominences that contribute to ulceration or discomfort.
- Blood flow restoration procedures: Revascularization techniques to improve circulation and enhance wound healing.
Your care team will assess your individual needs and recommend the most effective treatment plan, prioritizing limb preservation and optimal recovery.
Outcome
Limb salvage is a complex process, and long-term success requires a commitment to a healthier lifestyle. While no procedure can guarantee a permanent solution, the dedicated team in the Division of Vascular Surgery and Endovascular Therapy will collaborate closely with you, your family and your primary care provider to ensure the best possible outcome.
For many patients, our advanced limb salvage techniques can mean the difference between a minimally invasive procedure and the loss of an entire leg, offering hope and improved quality of life. Together, we are committed to preserving mobility and independence while minimizing the need for extensive interventions.
Clinical Trials
Our multidisciplinary team of vascular surgeons, podiatry specialists, biomechanical engineers and researchers are at the forefront of innovation, actively developing and testing cutting-edge techniques for the treatment of peripheral artery disease (PAD). Through collaborative research and advanced clinical practices, we aim to redefine care and improve outcomes for patients.
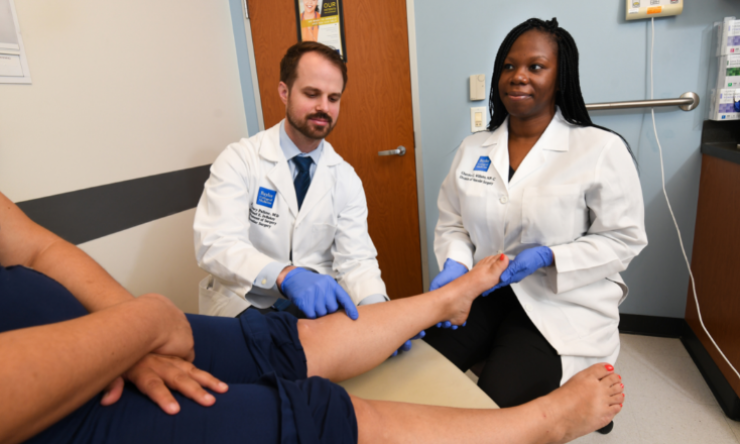
A second chance at life: Discovering an alternative to diabetic foot amputation
The Save the Extremity Program (STEP) at Baylor College of Medicine, founded by Dr. Joseph Mills uses the latest technology to save the limbs of diabetic patients.
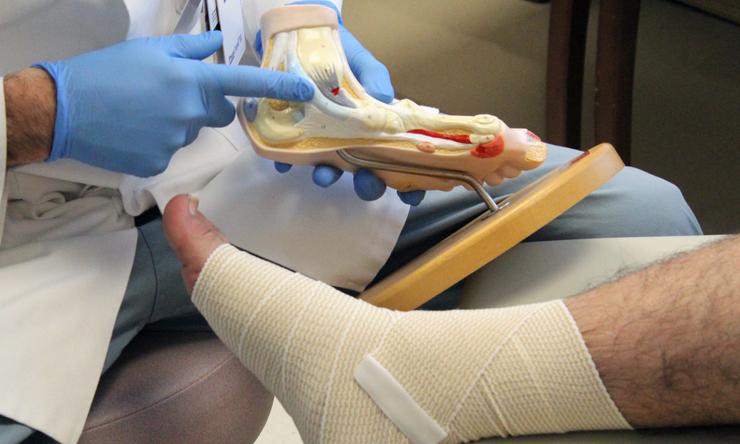
Tips for Diabetic Foot Care
Patients with diabetes lose feeling in their feet and are at risk for developing wounds that can become difficult to heal. This scenario is avoidable for many people through proper diabetic foot care.