Theme Leaders
Theme Description
Members of the CVRI Theme “Aortic, Vascular and Valvular Disease Research” lead a broad range of translational and clinical investigations spanning valvular heart disease, aortopathy, peripheral arterial disease, and hypertension. Their work focuses on defining the genetic, epigenetic, and molecular and cellular mechanisms underlying these conditions, as well as developing and evaluating novel medical, surgical, and device-based therapeutic strategies.
Current Clinical Projects
ATLAS (Applied Statistics and Machine Learning for the Advancement of Surgery)
The ATLAS platform takes a data-driven approach towards improving patient outcomes. ATLAS integrates large clinical datasets (eg, HCUP, NIS, NRD, STS and NTDB) with advanced machine learning algorithms to refine risk stratification, predict adverse events, and guide individualized treatment strategies for patients with complex aortic and valvular disease. By leveraging big-data analytics, ATLAS informs surgical decision-making and accelerates translational research across cardiovascular domains. Using publicly available data sets, ATLAS aims to apply advanced statistical theory to identify predictors of adverse events and define best-practice parameters in cardiothoracic surgery. The platform also serves as a collaborative data science hub for faculty and trainees, ensuring that insights from big data translate into actionable improvements in patient care.
- Training and support via office hours and an educational lecture series
- ATLAS enables surgeon-scientists to explore clinical data using artificial intelligence and machine learning
Valvular Heart Disease Outcomes and Robotic Surgery Research Program
The Valvular Heart Disease Research Program operates under the leadership of Dr. Kenneth K. Liao, Professor of Surgery and Chief of Cardiothoracic Transplantation and Mechanical Circulatory Support, and director of the Robotic Center for Cardiothoracic Surgery. Dr. Liao’s program is dedicated to advancing the field of valvular heart disease through innovative clinical research, translational collaborations, and the integration of cutting-edge surgical and transcatheter technologies. The mission of the program is to improve outcomes for patients with mitral, aortic, and tricuspid valve disease by leveraging minimally invasive and robotic surgical techniques, transcatheter valve therapies, left ventricular assist devices, and hybrid approaches for complex cases. Research priorities include the role of machine learning to refine risk stratification and guide individualized treatment and surgical techniques to better support heart transplant patients.
- First fully robotic heart transplant performed in the United States (March 2025)
- Milestone surpassing 800 robotic heart surgeries (September 2025)
Thoracic Aortic Aneurysms and Dissections
Our Thoracic Aortic Program leads international efforts to advance care for aneurysms and dissections through multi-center registries, clinical trials, educational lectures, and proprietary data analytics. Key registries include The International Registry for Acute Aortic Dissection, the Montalcino Aortic Consortium, and the Cardiothoracic Surgical Trials Network. We participate in numerous industry-sponsored randomized clinical trials involving aortic and valvular devices. Additionally, we coordinate a long-term, international multi-center observational study of Aortic Valve Operative Outcomes in Marfan Patients (AVOMP). We provide opportunities for investigator-initiated studies to surgeon-scientists using the proprietary Aortic Surgery Patient Database, which houses data from over 10,000 aortic interventions performed within the Division of Cardiothoracic Surgery. Ongoing study of clinical outcomes for a variety of aortic and valvular procedures captured in our proprietary database have resulted in several landmark publications elucidating complex surgical scenarios to better understand operative risk. Additionally, our faculty routinely participate in expert consensus clinical practice guidelines for a broad spectrum of valvular and aortic disease. These efforts define best practices, improve patient outcomes, and accelerate adoption of cutting-edge technologies.
- Aortic Valve Operative Outcomes in Marfan Patients
- Ongoing sponsored clinical trials ensure exposure to cutting-edge technology as new devices are developed to treat valvular and aortic disease.
Advanced Endovascular Aortic Research Program
Advanced Endovascular Aortic Research Program operates under the leadership of Dr. Gustavo S. Oderich, Professor of Surgery, Michael E. DeBakey Distinguished Endowed Chair in Surgery, Chief of Vascular Surgery and Endovascular Therapy, and Director of Baylor Medicine Center for Aortic Surgery. Dr. Ying Huang, as Program Director, is responsible for the execution, coordination, and oversight of all clinical research activities. The mission of the research program is to advance device-based therapies and improve both early and late outcomes for patients with aortic disease through rigorous physician-sponsored and industry-sponsored clinical trials, comparative-effectiveness studies, national and international multicenter prospective and retrospective observational registries, translational research, and quality-improvement initiatives – all grounded in a commitment to patient safety, equity, and rapid integration of evidence into clinical practice. The program’s research priorities include assessing the safety and effectiveness of novel endovascular and imaging technologies for complex aortic repair; conducting comparative analyses of outcomes following endovascular versus open aortic repair across a broad spectrum of patient risk profiles; optimizing perioperative management and long-term surveillance strategies to reduce aortic-related adverse events and reinterventions; strengthening national and international collaborations to better understand variations in outcomes across regions and healthcare systems; and building robust infrastructure for clinical and imaging data to support artificial-intelligence-driven research and innovation. In addition, the program collaborates with basic and translational science groups to develop and validate imaging, molecular, and genetic biomarkers that enhance risk stratification and guide individualized treatment selection.
- Clinical outcomes and quality of life measures in patients treated for complex abdominal, thoracoabdominal and aortic arch aneurysms or dissections with fenestrated and branched stent grafts
- United States aortic research consortium (US ARC) database
Vascular Surgery Outcomes and Peripheral Arterial Disease Research Program
The Vascular Surgery Outcomes and Peripheral Arterial Disease (PAD) Research Program operates under the leadership of Dr. Jayer Chung, M.D., MSc, Professor of Surgery and Principal Investigator, with key contributions from Dr. Cuneyt Koksoy and Dr. Ilse Torres. The program is dedicated to improving patient-centered outcomes for individuals with chronic limb-threatening ischemia (CLTI), acute limb ischemia (ALI), and other manifestations of peripheral arterial disease through rigorous clinical research, translational collaborations, and innovative technology integration. Our mission is to advance evidence-based care for patients with PAD by leveraging comparative effectiveness trials, national multicenter registries, artificial intelligence (AI) applications, translational projects, and wearable technology to optimize diagnosis, treatment, and long-term outcomes. We aim to reduce amputation rates, improve quality of life, and accelerate the translation of novel therapies into clinical practice. The program’s research priorities include comparative effectiveness trials of endovascular and open surgical interventions for CLTI and ALI. Via multi-center registries and industry collaborations, we prioritize the longitudinal assessment of wound healing, limb salvage, and amputation-free survival. In addition, we have several projects that aim to develop and validate AI-driven tools for angiographic image analysis and depression detection in PAD patients. In particular, we aim to integrate wearable-derived behavioral and physiologic data to predict outcomes and mental health status. Secondly, we aim to build a robust clinical and imaging database to support machine learning and predictive analytics to automate angiographic analysis. Finally, we aim to develop collaborative translational studies exploring molecular mechanisms of atherosclerosis, restenosis, and wound healing. The program maintains a longitudinal outcomes database of >900 CLTI patients and partners with leading institutions, including Rice University for AI and wearable technology research, and national collaborators through the Acute Limb Ischemia Research Consortium. Industry-sponsored trials (e.g., STRIDE II) and philanthropic support (Roderick D. MacDonald Fund, PATHS-UP Digital Health Seed Fund) further strengthen our research capacity.
- Association of wearable biomarkers and depression in chronic limb threatening ischemia (CLTI)
- National multicenter registry studying the comparative effectiveness of percutaneous versus open revascularization for acute limb ischemia (ALI)
- Development of patient-centric quality of life outcome metrics in chronic limb threatening ischemia (CLTI) and acute limb ischemia (ALI)
- Association of somatic mutations in atherosclerotic plaque and chronic limb threatening ischemia (CLTI)
- Utilization of the COMOS database to study epidemiological trends in acute limb ischemia (ALI) and chronic limb threatening ischemia (CLTI)
- Artificial intelligence models to automate the interpretation of angiographic data in chronic limb threatening ischemia (CLTI)
Current Basic Research Projects
Thoracic Aortic Aneurysm and Dissection
The Aortic Disease Research Laboratory at Baylor College of Medicine conducts basic and translational research on thoracic aortic aneurysms and dissections. The laboratory aims to define the molecular mechanisms that drive disease initiation and progression and to identify therapeutic targets that can prevent aortic degeneration. The laboratory investigates dynamic changes in signaling pathways, epigenetic regulation, aortic cell phenotypic transitions, and inflammatory responses that shape aortic injury, repair, and remodeling. The research integrates human tissue and biomarker analyses, multiple clinically relevant mouse models of aortic disease, detailed aortic structural and biomechanical assessments, and mechanistic cell-culture systems. The laboratory leverages a broad range of molecular and cellular approaches, with particular emphasis on single-cell omics platforms, including scRNA-seq, scATAC-seq, and spatial transcriptomics, to resolve cell-type–specific and spatially organized mechanisms underlying aortic pathology. The laboratory also houses the Human Thoracic Aortic Disease Tissue Bank, which contains blood samples, aortic tissues, and detailed phenotypic information from more than 4,500 patients with aortic aneurysms or dissections. This extensive biorepository provides an unparalleled resource for comprehensive investigation of the genetic, epigenetic, molecular, and cellular determinants of thoracic aortic disease across diverse patient populations.
- Epigenetic Regulation of Trained Immunity in Thoracic Aortic Aneurysms and Dissections
- Endothelial Dysfunction in the Development of Aortic Degeneration, Dissection, and Rupture
- Cellular and Molecular Drivers of Acute Aortic Dissections
- Pro-inflammatory Pyroptotic Cell Death in Aortic Degeneration
- Mitochondrial Damage Induced Programmed Cell Death in Sporadic Ascending Thoracic Aortic Aneurysm and Dissection
Faculty
- Lauren Barron, M.D. – Surgery – Cardiothoracic Surgery; Complex aortic and valve surgery, especially aortic root replacement, alternative access transcatheter valve replacement (TAVR), patient optimization for surgery
- Neal Barshes, M.D., MPH – Surgery – Vascular Surgery & Endovascular Therapy; Peripheral vascular disease, diabetes mellitus
- Jeffrey T. Bates, M.D. – Medicine – Cardiovascular Research; General Internal Medicine, Vascular Medicine, Hypertension
- Subhasis Chatterjee, M.D. - Surgery – Cardiothoracic Surgery; Critical management of cardiovascular patients, practice guidelines, application of artificial intelligence and machine learning to clinical outcomes. Enhanced recovery pathways. ECMO and Mechanical Circulatory Support.
- Jayer Chung, M.D. – Surgery – Vascular Surgery & Endovascular Therapy; Cardiovascular disease, especially acute limb ischemia, coronary artery disease, and peripheral vascular disease
- Lorraine Cornwell, M.D. – Surgery – Cardiothoracic Surgery; TAVR, optimization of clinical outcomes of cardiothoracic surgery, especially minimally invasive procedures, off-pump CABG, valve repair, and VATS lobectomy
- Joseph Coselli, M.D. – Surgery – Cardiothoracic Surgery; Complex aortic open surgical and endovascular repair, especially the aortic root, aortic arch, and thoracoabdominal aorta, clinical outcomes, Marfan syndrome
- Heather Dickerson, M.D. – Pediatrics – Cardiology and Cardiac Critical Care; Pediatric cardiac critical care, including ventricular assist devices and extracorporeal membrane oxygenation, pediatric cardiology with a focus in echocardiography and single ventricle cardiac lesions
- Ravi Ghanta, M.D. – Surgery – Cardiothoracic Surgery; Aortic and valve surgery, ventricular remodeling in cardiac failure, CABG, tissue engineering, application of artificial intelligence and machine learning to clinical outcomes
- Ying Huang, M.D, Ph.D. – Surgery – Vascular Surgery & Endovascular Therapy; Clinical researcher in cardiovascular and vascular diseases with a focus on advanced endovascular aortic repair, investigational device exemption device (IDE) clinical trials and research for complex aortic aneurysms, clinical guidelines, and expertise in clinical research methodology, biostatistics, and data science
- Cuneyt Koksoy, M.D. – Vascular Surgery - PAD outcomes research, multicenter registry coordination, sex-stratified analyses in ALI, advanced imaging interpretation, and translational collaborations in wound healing and atherosclerosis
- Srikanth Koneru, M.D. – Medicine – Cardiology; Structural Interventional Imaging, Cardiac CT and MRI Imaging, Cardio-Oncology and Strain Imaging, General Cardiology, Valvular Heart Disease, Disease of Aorta, Echocardiographic guided AV Optimization, HOCM, Cardiomyopathy
- Veronica Lenge De Rosen, M.D. – Radiology – Cardiothoracic Imaging; Imaging of coronary vasculature, imaging of ischemic and non-ischemic cardiomyopathy, imaging of lung and pleural malignancy, lung transplant, and interstitial lung disease
- Yanming Li, Ph.D. – Surgery – Cardiothoracic Surgery; Mechanisms for aortic aneurysm and dissection, advanced computational analysis
- Kenneth K. Liao, M.D., Ph.D. – Surgery – Minimally invasive and robotic cardiac surgery, Minimally invasive and robotic mitral valve repair/replacement, Minimally invasive and robotic aortic valve repair/replacement, robotic coronary artery bypass, Heart and lung transplantation, Ventricular assist device (VAD), Aortic aneurysm repair, Transcatheter aortic valve replacement (TAVR) and mechanical circulatory support
- Steve Maximus, M.D. – Surgery – Vascular Surgery & Endovascular Therapy – Thoracoabdominal aortic aneurysms and dissections, fenestrated and branched endovascular aortic repair, endovascular repair of aortic arch aneurysms and dissections, physician modified endografts (PMEG)
- Thanila de Araujo Macedo, M.D, MBA – Radiology - Vascular Surgery & Endovascular Therapy; Advanced Aortic Imaging Techniques including Contrast Enhanced Ultrasound (CEUS), 4D Computed Tomography Angiography (CTA) and integrated Artificial Intelligence (AI)-driven analysis of imaging data
- Joseph Mills, M.D. – Surgery – Vascular Surgery & Endovascular Therapy; Approaches to reduce diabetes-related lower extremity amputation
- Tamer Mohamed, Ph.D. – Surgery – Cardiothoracic; Endogenous heart repair and cardiac regeneration
- Marc Moon, M.D. – Surgery – Cardiothoracic Surgery; Complex aortic and valve surgery, especially repair of the mitral valve and aortic repair during pregnancy, TAVR, CABG, arrhythmia ablation
- Shaine Morris, M.D., MPH – Pediatrics – Cardiology; Advanced imaging techniques for genetically triggered aortopathy
- Gustavo S. Oderich, M.D. – Surgery – Vascular Surgery & Endovascular Therapy – Open and endovascular repair of aortic disease, including fenestrated and branched endovascular repair, with experience across arterial and venous beds such as carotid, visceral, and peripheral vessels. Global principal investigator for Cook investigational device exemption device (IDE) clinical trial, with clinical research focus on advanced endovascular and imaging technologies applied to complex endovascular aortic repair and artificial intelligence (AI)-driven clinical research
- Vicente Orozco-Sevilla, M.D. – Surgery – Cardiothoracic Surgery; Complex aortic open surgical and endovascular repair, hybrid repair approaches, clinical outcomes
- Wei Pan, M.D. – Anesthesiology – Cardiothoracic Surgery; Autologous blood transfusion during complex aortic repair, temperature management during hypothermic circulatory arrest, cerebrospinal fluid drainage
- Todd Rosengart, M.D. – Surgery – Cardiothoracic Surgery; off-pump surgery, minimally invasive aortic, coronary and valvular surgery, mitral valve repair or replacement
- Ying Shen, M.D. – Surgery – Cardiothoracic Surgery; Mechanisms for aortic aneurysm and dissection
- Guilherme Vianna Silva, M.D. – Medicine – Cardiology; Transcatheter treatments for valvular disease
- Ana Maria Segura, M.D., MPH - Pathology – Cardiovascular Pathology; Heart failure, ventricular remodeling, transplantation, ventricular assist devices, aortic pathology and electrophysiology
- Addison Taylor, M.D., Ph.D. – Medicine – Hypertension; Hypertension, clinical pharmacology
- Ilse Torres, M.D. – Surgery - Vascular Surgery; Acute limb ischemia management, thrombotic burden analysis, clinical trial participation, and quality-of-life outcomes research
- Deborah C. Vela, M.D., MS - Pathology – Cardiovascular Pathology; Atherosclerosis, aortic aneurysm and dissection, peripheral vascular disease, and myocardial infarction
- Anna H. Xue, M.D. - Surgery – Cardiothoracic Surgery; Complex open aortic surgery, acute type A aortic dissection, and Marfan syndrome
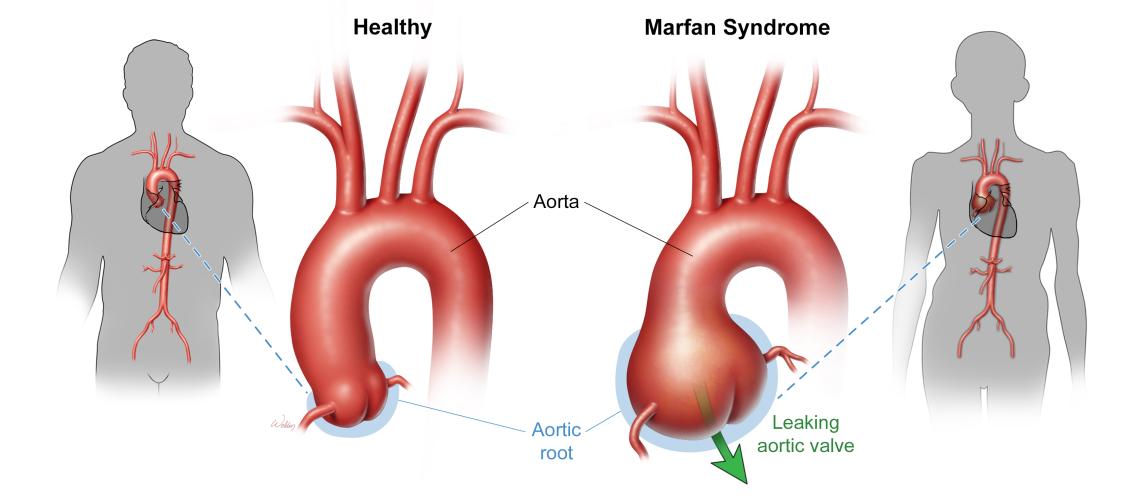
Illustration of a normal aorta root seen in a healthy individual (left) and a dilated aorta root causing aortic valve leakage in a patient with Marfan syndrome.
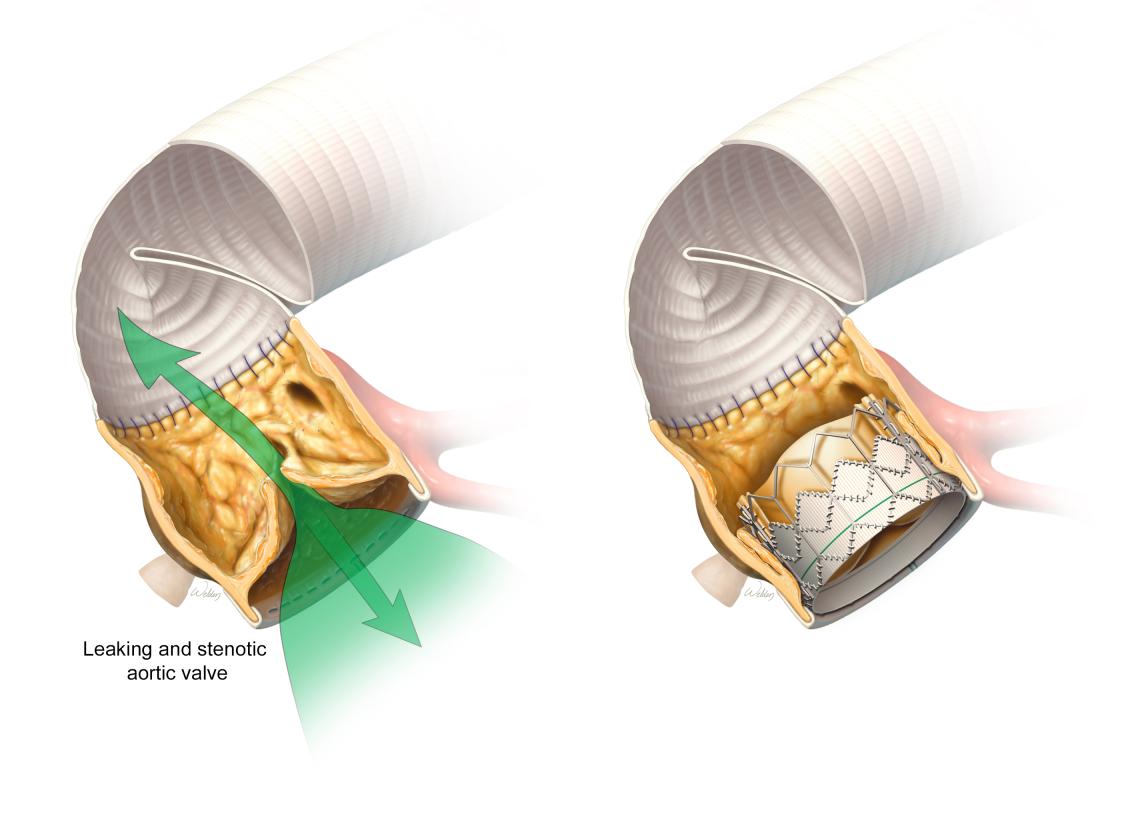
Illustration of an innovative valve-in-valve approach to address a late valvular complication in a patient with prior aortic root replacement using a porcine bioprosthetic root (left). In lieu of a repeat sternotomy to fix the degenerated aortic valve, transcatheter aortic valve replacement (TAVR) was performed endovascularly, placing the device within the older valve (right).

