Overview
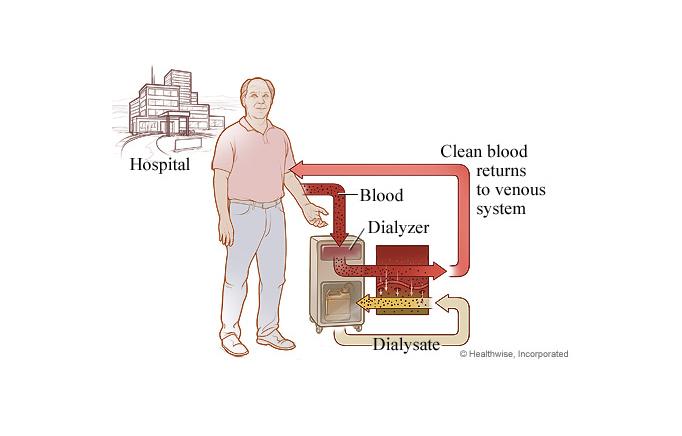
Chronic kidney disease and acute kidney injury (also known as acute renal failure) cause the kidneys to lose their ability to filter and remove waste and extra fluid from the body. Hemodialysis is a process that uses a man-made membrane (dialyzer) to:
Remove wastes, such as urea, from the blood.Restore the proper balance of electrolytes in the blood.Eliminate extra fluid from the body.
For hemodialysis, you are connected to a filter (dialyzer) by tubes attached to your blood vessels. Your blood is slowly pumped from your body into the dialyzer, where waste products and extra fluid are removed. The filtered blood is then pumped back into your body.
There are different types of hemodialysis. Talk about these with your doctor to decide which one might be best for you.
In-center hemodialysis
You go to a hospital or a dialysis center. Hemodialysis usually is done 3 days a week and takes 3 to 5 hours a day.
Home hemodialysis
After you are trained, you do your dialysis treatments at home. Hemodialysis is usually done 3 days a week (or every other day). Discuss with your doctor how long each session needs to be. A session could be as long as 6 hours, which may help you feel better.
Daily home hemodialysis
After you are trained, you do your dialysis treatments at home. Hemodialysis is done 5 to 7 days a week. Each session takes about 3 hours.
Nocturnal home hemodialysis
After you are trained, you do your dialysis treatments at home. Hemodialysis is done 3 to 7 nights a week. Each session is done overnight (about 6 to 8 hours).
Before treatments can begin, your doctor will need to create a site where the blood can flow in and out of your body during the dialysis sessions. This is called the dialysis access. The type of dialysis access you have will depend in part on how quickly you need to begin hemodialysis.
There are different types of access for hemodialysis
Fistula
A fistula is created by connecting an artery to a vein in your lower arm. A fistula allows repeated access for each dialysis session. It may take several months for the fistula to form. A fistula may not clot as easily as other dialysis access methods. A fistula is the most effective dialysis access and the most durable. Complications include infection at the site of access and clot formation (thrombosis).
Graft
A vascular access that uses a synthetic tube implanted under the skin in your arm (graft) may be used if you have very small veins. The tube becomes an artificial vein that can be used repeatedly for needle placement and blood access during hemodialysis. A graft does not need to develop as a fistula does, so a graft can sometimes be used as soon as 1 week after placement. Compared with fistulas, grafts tend to have more problems with clotting or infection and need to be replaced sooner. A polytetrafluoroethylene (PTFE or Gore-Tex) graft is the most common type used for hemodialysis.
Venous catheter
A tube, or catheter, may be used temporarily if you have not had time to get a permanent access. The catheter is usually placed in a vein in the neck, chest, or groin. Because it can clog and become infected, this type of catheter is not routinely used for permanent access. But if you need to start hemodialysis right away, a catheter may be used until your permanent access is ready.
Hemodialysis for acute kidney injury may be done daily until kidney function returns.
Choosing between treatment with hemodialysis or peritoneal dialysis is based on your lifestyle, other medical conditions, and body size and shape. Talk to your doctor about which type would be best for you.
© 2016-2019 Healthwise, Incorporated.
What Is a Hemodialysis Access?
Hemodialysis is a treatment that removes wastes and extra fluid from your blood when your own kidneys have failed. Before hemodialysis can be done, a connection must be made to the blood inside your blood vessels. Your hemodialysis access, or vascular access, is a way to reach your blood for hemodialysis. The access allows your blood to travel through soft tubes to the dialysis machine where it is cleaned as it passes through a special filter, called a dialyzer.
Are Different Types of Vascular Access Available?
There are three different types of access can be placed for hemodialysis. They are called a fistula, a graft and a catheter. Your doctor should teach you about the advantages and disadvantages of each one. Your doctor should refer you to a special surgeon with hemodialysis access experience at least six months before you need to start treatment. This surgeon will evaluate you and help you choose the type of access that is best for you. Once your doctor tells you that you will need dialysis, you should protect the arm where the surgery will be done. Don't allow anyone to draw blood or give you an injection in this arm. Also, never let anyone use a cuff to take your blood pressure from this arm. You should wear a medical alert bracelet to inform hospital staff about your arm.
Fistula. A fistula is the best choice for hemodialysis. It is preferred because it usually lasts longer and has fewer problems like clotting and infections. A fistula should be placed several months before you need to start dialysis. This allows the fistula enough time to be ready when you need treatment. Minor surgery is needed to create a fistula. It is made by connecting a vein to a nearby artery, usually in your arm. This creates a large blood vessel that has a fast flow of blood. Your wrist or elbow is the preferred location for your fistula. A fistula will usually last for many years. A fistula usually takes one to four months to "mature" or enlarge before it can be used. If you are already receiving hemodialysis using a graft or catheter, ask your doctor about the benefits of a fistula.
Graft. A graft is the second choice for an access. Minor surgery is done using an artificial tube between a vein and a nearby artery. A graft is usually put inside the bend of your arm or in your upper arm. Sometimes, grafts may be placed in your leg or chest wall. Grafts generally need to be in place at least two weeks after surgery before they can be used.
Catheter. Catheters are most often used for a temporary access. For example, they are sometimes used for a short time in people who get a fistula and need to start dialysis before the fistula is ready. Once the fistula is "mature," the catheter will be removed. Sometimes a catheter is used over a long period of time because a fistula or graft is not possible. Catheters are made of soft plastic tubing. There are two parts, one for removing your blood and the other for returning the cleaned blood to your body. Catheters are placed only when you need to start dialysis. They are put in a large vein, usually in your neck but sometimes in your upper chest. Catheters have more problems (like clotting and infections) than fistulas or grafts. They may not have enough blood flow for good dialysis treatment.
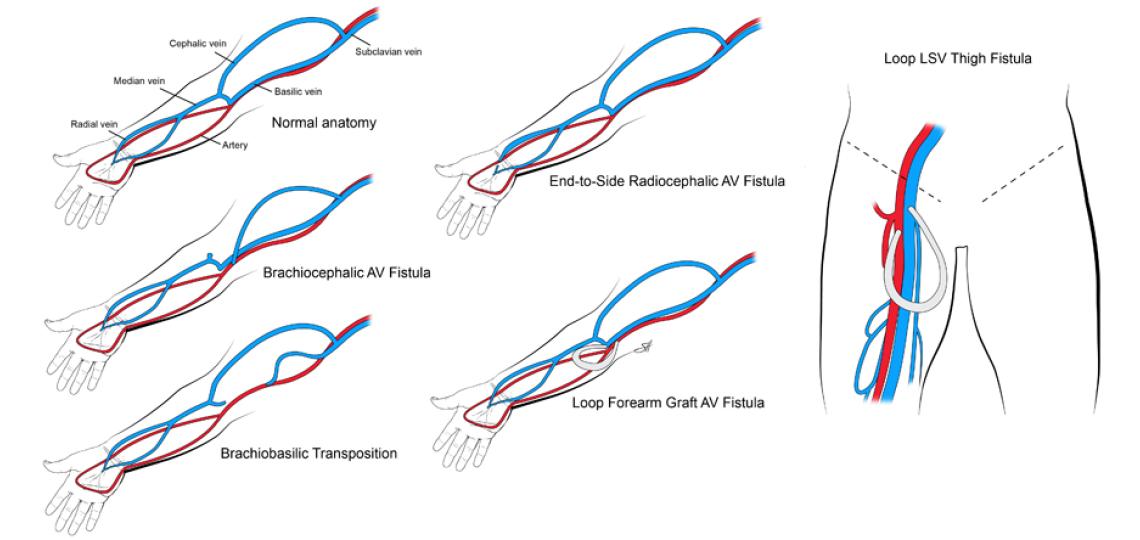
Illustration of types of vascular access for dialysis which include fistula, graft and catheter
What Kind of Anesthesia Is Used for a Dialysis Operation Performed and What Is the Recovery Time?
A dialysis access operation, either an AV fistula or AV graft, can be performed under either local or general anesthesia. The operation typically takes about two hours.
After recovering in the recovery room, the patient can go home. There will be a sterile, transparent dressing on the incision. The dressing can be taken off at home after 72 hours and the incision left uncovered. It is okay to shower normally with the uncovered incision.
The stitches are absorbable and will not need to be removed. You will be seen in the clinic approximately two weeks following surgery. Generally it takes at least four to six weeks to allow an AV fistula or graft to be ready for dialysis access.
What Happens During a Dialysis Procedure?
If a patient has a working dialysis access as either a fistula or graft, dialysis can be initiated. In this process, two needles are inserted into dialysis access at the beginning of each dialysis. These needles are connected to soft plastic tubes that go to the dialysis machine. The patient's blood travels to the machine through one of these tubes. The blood passes through the dialyzer, or artificial kidney, where it is cleaned. It is returned back to the patient through the other tube. If a patient has a catheter, it can be connected directly to the dialysis tubes, and no needles are used.
What Happens During a Dialysis Procedure?
If a patient has a working dialysis access as either a fistula or graft, dialysis can be initiated. In this process, two needles are inserted into dialysis access at the beginning of each dialysis. These needles are connected to soft plastic tubes that go to the dialysis machine. The patient's blood travels to the machine through one of these tubes. The blood passes through the dialyzer, or artificial kidney, where it is cleaned. It is returned back to the patient through the other tube. If a patient has a catheter, it can be connected directly to the dialysis tubes, and no needles are used.
What Are the Potential Risks for a Dialysis Access Operation?
As with any intervention or operation, one has to be aware of the risks of the operation. The risks of anesthesia are minimized, due to the fact that this is under local anesthesia with sedation; but the risk is not zero. There is always a possibility of the fistula or graft clotting, but the risk is lower with a fistula than a graft.
Sometimes, particularly in diabetic patients, the fistula can "steal" blood away from the hand. If this happens, one has to watch for hand or finger pain, numbness and tingling, and in the worst situations, a reduction in the strength and/or sensation in the hand. If these symptoms occur, it is important for you to let the surgeon know about it. It may occasionally require additional surgery to prevent the symptoms from worsening, and in the extreme circumstance, it may require tying off the fistula or the graft.
The other potential risk is that one can develop an infection in the skin, which is most times easily treated with antibiotics. Rarely, months or years later the graft can get infected, in which case it has to be removed. The risk of this is much lower with a fistula than with a graft.
It is important to realize that the term "permanent dialysis access" is not accurate because many times patients with renal failure will require an additional operation or operations. However, if one has a functioning fistula, the chance of this is much lower than with a graft. With advanced planning, however, a good functional access can be obtained in the majority of patients.