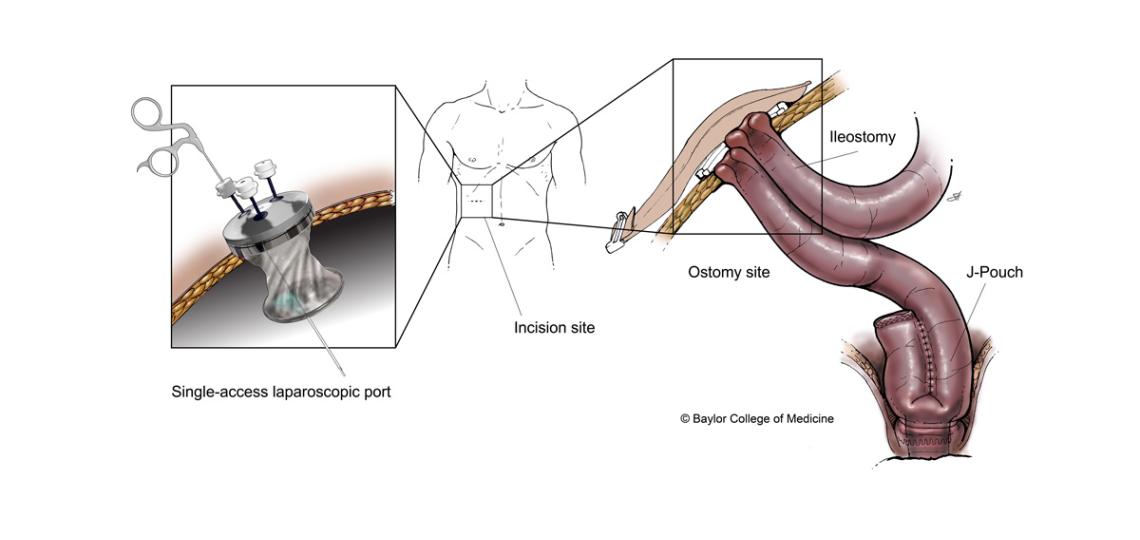
An ileostomy is a surgical procedure that is used when the lower part of the digestive system (the colon) is diseased or damaged and is not able to function normally. An ileostomy allows body waste to leave the body through a surgical opening.
In this procedure, a hole is made in the abdomen. Then a portion of the small intestine (the ileum) is brought to an opening in the skin (a stoma). Waste leaves the body through the stoma instead of the anus. The waste is collected in a pouch attached to the stoma with adhesive.
Ileostomies may be done if all of the colon is removed or diseased, such as from ulcerative colitis or Crohn's disease.
Surgeries that may require an ostomy
An ileostomy may be used for a short or long time.
When your ileostomy is short-term, it usually means all of your large intestine was removed but you still have at least part of your rectum.
If you have surgery on part of your large intestine, your doctor may want the rest of your intestine to rest for a while. You will use the ileostomy while you recover from this surgery. When you do not need it anymore, you will have another surgery to reattach the ends of the small intestine, and you will no longer need the ileostomy.
You will need to use it long-term if all of your large intestine and rectum have been removed.
To create the ileostomy, the surgeon makes a small surgical cut in the wall of your belly. Part of your small intestine that is farthest from your stomach is brought up and used to make an opening, called a stoma. When you look at your stoma, you are actually looking at the lining of your intestine. It looks a lot like the inside of your cheek.
Sometimes, an ileostomy is done as the first step in forming an ileal-anal reservoir (called a J-pouch).
What happens before your ileostomy surgery?
Surgery can be stressful. This information will help you understand what you can expect. And it will help you safely prepare for surgery.
Preparing for surgery
Understand exactly what surgery is planned, along with the risks, benefits, and other options.
Tell your doctors ALL the medicines, vitamins, supplements, and herbal remedies you take. Some of these can increase the risk of bleeding or interact with anesthesia.
If you take blood thinners, such as warfarin (Coumadin), clopidogrel (Plavix), or aspirin, be sure to talk to your doctor. He or she will tell you if you should stop taking these medicines before your surgery. Make sure that you understand exactly what your doctor wants you to do.
Your doctor will tell you which medicines to take or stop before your surgery. You may need to stop taking certain medicines a week or more before surgery. So talk to your doctor as soon as you can.
If you have an advance directive, let your doctor know. It may include a living will and a durable power of attorney for health care. Bring a copy to the hospital. If you don’t have one, you may want to prepare one. It lets your doctor and loved ones know your health care wishes. Doctors advise that everyone prepare these papers before any type of surgery or procedure.
You may need to go to the hospital the day before surgery to prepare your colon. You will get laxatives to completely empty your colon.
How can you care for yourself after an ileostomy?
Activity
Rest when you feel tired. Getting enough sleep will help you recover.
Try to walk each day. Start by walking a little more than you did the day before. Bit by bit, increase the amount you walk. Walking boosts blood flow and helps prevent pneumonia and constipation.
Avoid strenuous activities, such as bicycle riding, jogging, weight lifting, or aerobic exercise, until your doctor says it is okay. When you are active again, a support belt can help secure the ileostomy pouch.
Ask your doctor when you can drive again.You will probably need to take 4 to 6 weeks off from work. It depends on the type of work you do and how you feel.
Your doctor will tell you when you can shower after surgery. You can shower with or without the ileostomy pouch. You do not need to worry about getting soap or water inside the tube.Your doctor will tell you when you can have sex again. You may feel uncomfortable about sex after an ileostomy. Talk to your doctor if you have problems. You can get special underclothing that hides the pouch during sex.
Diet
You may not have much appetite after the surgery. But try to eat a healthy diet.
Eat a low-fiber diet for several weeks after surgery. It is best to eat many small meals throughout the day. Add high-fiber foods a little at a time. You may need to take vitamins that contain sodium and potassium. Ask your doctor.
Drink plenty of fluids to avoid becoming dehydrated.
Medicines
Your doctor will tell you if and when you can restart your medicines. He or she will also give you instructions about taking any new medicines.
If you take blood thinners, such as warfarin (Coumadin), clopidogrel (Plavix), or aspirin, be sure to talk to your doctor. He or she will tell you if and when to start taking those medicines again. Make sure that you understand exactly what your doctor wants you to do.
Take pain medicines exactly as directed. If the doctor gave you a prescription medicine for pain, take it as prescribed.
If you are not taking a prescription pain medicine, ask your doctor if you can take an over-the-counter medicine.
If your doctor prescribed antibiotics, take them as directed. Do not stop taking them just because you feel better. You need to take the full course of antibiotics.
Your doctor will tell you if you need to take some medicines in a different form now that you have a stoma. You may need to crush pills or take a liquid form of the medicine.
Other instructions
If the skin under your pouch is red, irritated, or itchy, you need to treat your skin. Follow these steps:
- Gently remove the pouch.
- Clean the skin under the pouch with water.
- Dry the skin.
- Sprinkle ostomy protective powder on the skin, and then blot it off.
- Reattach or replace the pouch.
If you continue to have skin irritation, consult your wound, ostomy, and continence nurse (WOCN) or other health professional.
© 2016-2019 Healthwise, Incorporated.
Ostomy Care
Information on how to care for an ostomy.