For over 15 years, we at the Office of Outreach and Health Disparities in the Dan L Ducan Comprehensive Cancer Center at Baylor College of Medicine have been committed to addressing cancer disparities by creating a broad collection of evidence-based educational resources aimed to inform and support medically underserved, minority, and diverse populations. Many of these educational resources have been developed in partnership with organizations from the Community Network for Cancer Prevention (CNCP) and are integrated into the clinical practice of CNCP members. These materials are utilized by our healthcare partners, including Harris Health, San Jose Clinic, Tomagwa Healthcare Ministries and other community clinics, to enhance their cancer prevention efforts. Each resource is culturally and linguistically tailored to meet the needs of Black or African American, non-Hispanic White, Hispanic, and Vietnamese communities. We are grateful to the Cancer Prevention and Research Institute of Texas (CPRIT) for funding throughout the years the development and implementation of many of the educational materials presented here.
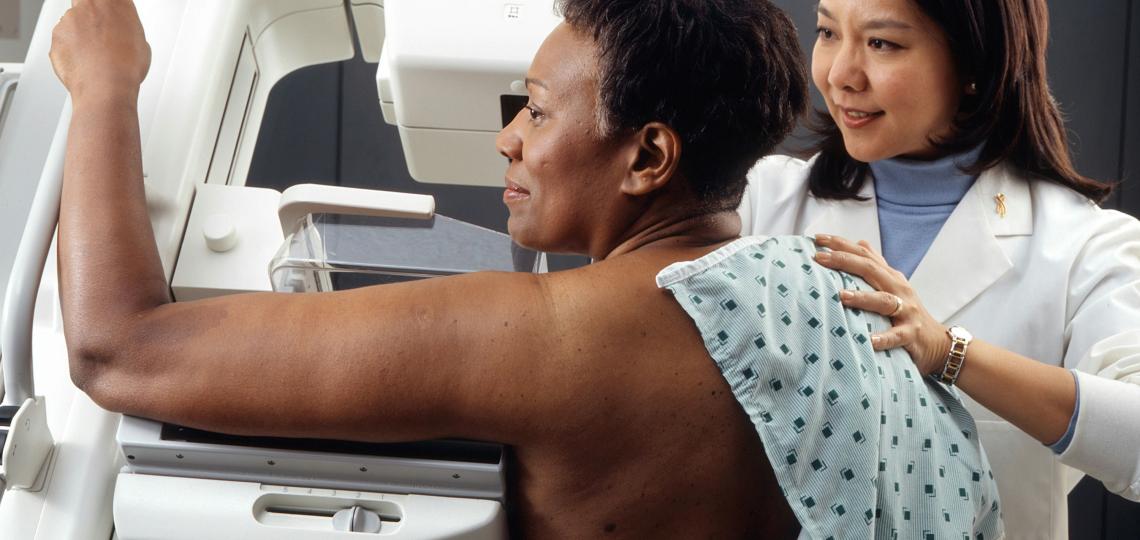
Breast Cancer Screening and Education
Breast cancer is the second most common cancer among women in the United States and it is one of the leading causes of cancer-related deaths. Breast cancer may be detected early with regular screening. Screening can prevent breast cancer by finding abnormal changes in the cells or cancerous tumors of the breast that can be treated before it spreads to other parts of the body. When breast cancer is detected early, it increases the chances of successful treatment.
The American Cancer Society recommends that women with an average risk of breast cancer start screening at age 45. Women should be screened yearly until they are age 54. Women age 55 and older should speak with their doctor to decide if they should continue to get screened every year or every other year.
The American Cancer Society also recommends that women with a higher risk of developing breast cancer should start screening earlier at age 30. These individuals include those with known BRCA1 or BRCA2 gene mutations, first-degree relatives (i.e., parents, siblings, children) with a gene mutation, radiation therapy of the chest before age 30, Li-Fraumeni syndrome, Cowden syndrome, Bannayan-Riley-Ruvalcaba syndrome, or have first-degree relatives with one of those syndromes.
Please visit the American Cancer Society website for additional information on breast cancer screening exams and breast cancer screening guidelines.
Colorectal Cancer Screening and Education
Colorectal cancer (CRC) is one of the most common cancers in the United States and is the second leading cause of cancer-related deaths. CRC may be detected with regular screening. Screening tests are important because they can help prevent CRC by detecting precancerous growths (known as polyps) in the colon or rectum or help detect the cancer early when it’s small and hasn’t spread. When CRC is detected early, it can be easily treated.
The American Cancer Society and other organizations have developed screening guidelines for people at average and high risk for colorectal cancer. Men and women who are 45 years of age and older should be regularly screened for colorectal cancer. Some individuals with higher risk need to be tested at an earlier age. According to the American Cancer Society, individuals who have certain intestinal diseases (ulcerative colitis and Crohn’s disease), inheritable colon cancer syndromes (familial adenomatous polyposis and Lynch syndrome) are at high risk of colorectal cancer and should begin screening at even younger age.
Selected Colorectal Cancer Screening Tests

Cervical Cancer Screening and Education
Cervical cancer is caused by changes to the healthy cells in the cervix. Regular screening can find abnormal cells in the cervix early so doctors can treat them before turning into cancer. When cervical cancer is detected early, it can often be treated successfully.
Cancer Education Resource Websites
The following is a listing of useful websites to learn more about breast, colorectal, cervical cancer and HPV education.








