
Our lab's vision is “bringing artificial intelligence to the bedside.”
About the Lab
What is Artificial Intelligence
Artificial Intelligence (AI) is an umbrella term to describe computers and technology to simulate intelligent behavior and critical thinking comparable to a human being[1]. AI is not one technology but rather a collection of them: machine learning (neural networks and deep learning), natural language processing, rule-based expert systems, physical robots, and robotic process automation[2]. Since the Turing machine, AI is already being utilized in the medical field: diagnosis and treatment applications, patient engagement and adherence applications, administrative applications, and implications for the healthcare workforce. Most AI models remain within the testing and prototyping environment; only a handful was utilized in clinical practice as clinical decision support [3]. The main concerns/barriers for implementing AIs are data management, the development of models, or the implementation in the (clinical) workflow.
Academic Leader in Clinical Data Science
Our ultimate goal is to become an academic leader in clinical data science, with focused on using multidisciplinary sciences (health information technology and clinical research) to improve the outcomes of healthcare. The AIH Lab will be at the center of interactions between unmet clinical needs and the advanced, innovative machine learning techniques. Our research will translate novel AI into interpretable, applicable tools as clinical decision aids.
Our lab will be well-placed to fill the gap identified in a 2018 JAMA publication which highlighted that machine learning approaches will transform all aspects of medicine and health care, but to date this transformation remains largely aspirational.”[1] The author stated that, in clinical settings, there is an unmet need for accurate and interpretable predictive models to further improve clinical care rather than complicate this process.
Currently, electronic health records (EHR) provide the deepest array of clinical data from outpatient encounters to inpatient visits and machine learning algorithms have the potential to:
- Create models that accurately classify a patient’s diagnosis
- Predict what a patient may experience in the future
- Reveal the phenotype of diseases
- Provide answers to who may benefit the most from interventions
Our contributions to clinical data science will be the integration of quantitative models using EHR data to a clinical decision aid at the point of care.
Location
Our lab is located in two centers: ICTR and IQuESt. We benefit from collaborating with the Institute for Clinical and Translational Research (ICTR) at Baylor College of Medicine and Center for Innovations in Quality, Effectiveness and Safety (IQuESt) at the Michael E. DeBakey VA Medical Center (MEDVAMC).
Cited Publications
- Rivara, F.P., S.D. Fihn, and R.H. Perlis, Advancing Health and Health Care Using Machine Learning: JAMA Network Open Call for Papers. JAMA network open, 2018. 1(8): p. e187176-e187176.
- Amisha, P.M., M. Pathania, and V.K. Rathaur, Overview of artificial intelligence in medicine. Journal of family medicine and primary care, 2019. 8(7): p. 2328.
- Davenport, T. and R. Kalakota, The potential for artificial intelligence in healthcare. Future healthcare journal, 2019. 6(2): p. 94.
- van de Sande, D., et al., Moving from bytes to bedside: a systematic review on the use of artificial intelligence in the intensive care unit. Intensive care medicine, 2021: p. 1-11.
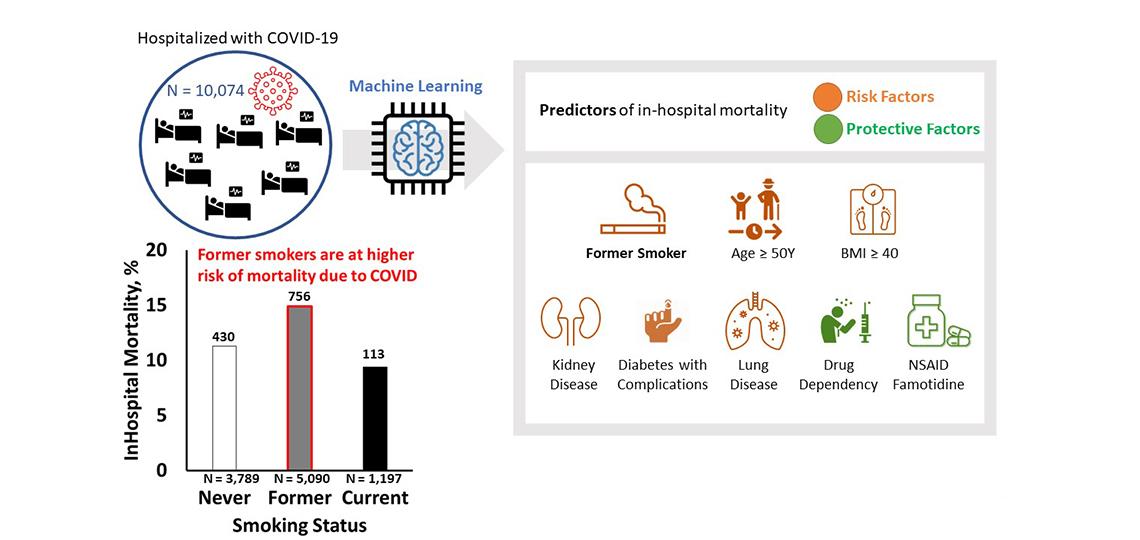
We observed that former smokers are at the elevated risk of COIVD-19 severity of illness.
Razjouyan J, Helmer DA, Lynch KE, Hanania NA, Klotman PE, Sharafkhaneh A, Amos CI. Smoking Status and Factors associated with COVID-19 In-hospital Mortality among U.S. Veterans. Nicotine Tob Res.
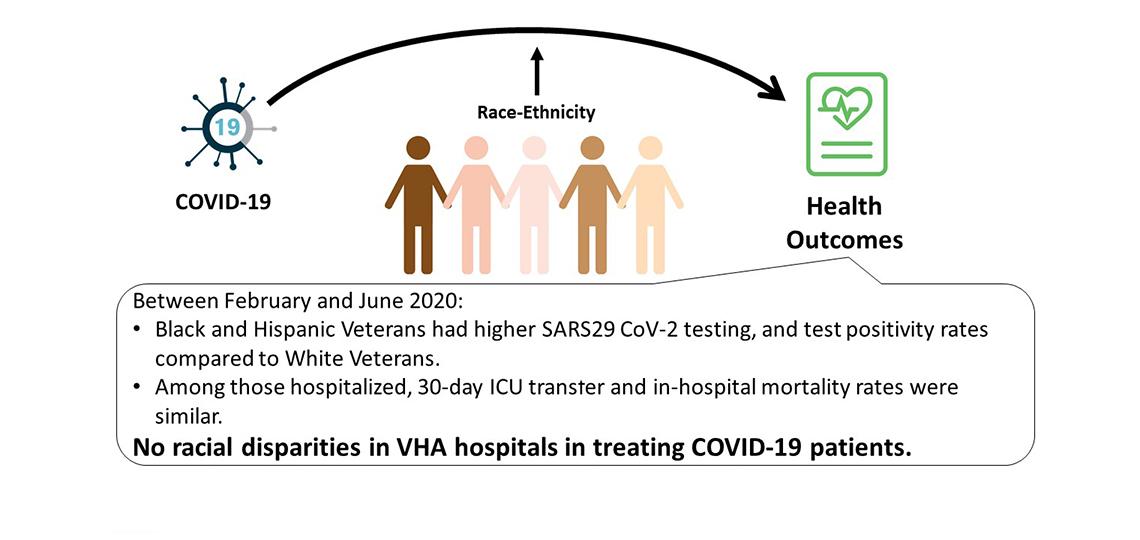
No racial disparities in VHA hospitals in treating COVID-19 patients.
Razjouyan J, Helmer DA, Li A, Naik AD, Amos CI, Bandi V, Sharafkhaneh A. Differences in COVID-19-Related Testing and Healthcare Utilization by Race and Ethnicity in the Veterans Health Administration. J Racial Ethn Health Disparities.
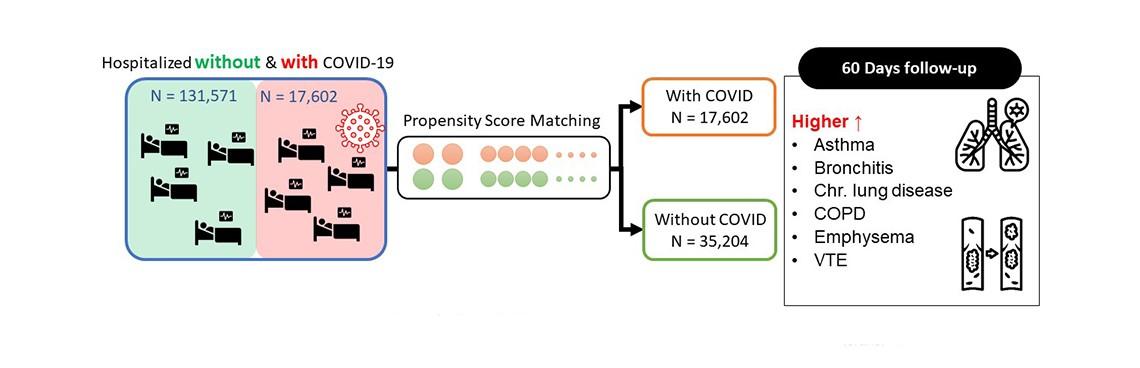
COVID-19 positive patients has higher respiratory disease 60-day post index date of hospitalization.
Park, C.; Razjouyan, J.; Hanania, N.A.; Helmer, D.A.; Naik, A.D.; Lynch, K.E.; Amos, C.I.; Sharafkhaneh, A. Elevated Risk of Chronic Respiratory Conditions within 60 Days of COVID-19 Hospitalization in Veterans. Healthcare 2022.
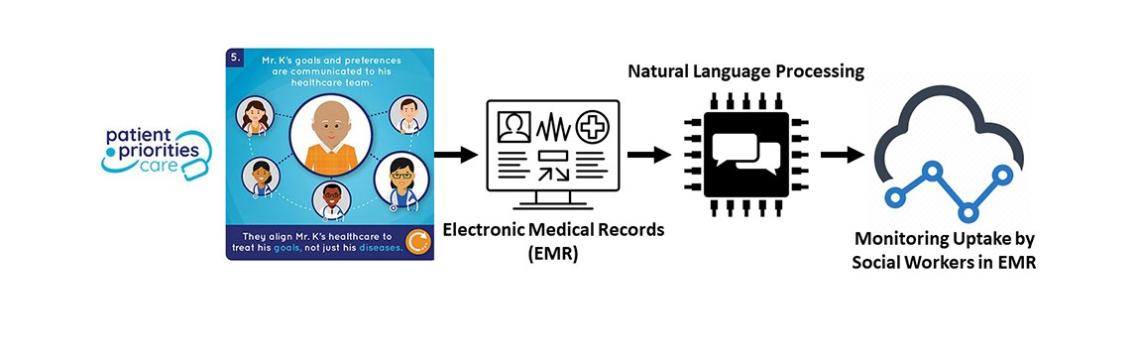
We implement an NLP tool to monitor the uptake of interventions among social workers.
Razjouyan J, Freytag J, Dindo L, Kiefer L, Odom E, Halaszynski J, Silva JW, Naik AD. Measuring Adoption of Patient Priorities-Aligned Care Using Natural Language Processing of Electronic Health Records: Development and Validation of the Model. JMIR Med Inform.
Zimolzak AJ, Shahid U, Giardina TD, et al. Why Test Results Are Still Getting "Lost" to Follow-up: a Qualitative Study of Implementation Gaps. J Gen Intern Med. 2022 Jan;37(1):137-144. PMID: 33907982
Alkhairy S, Celi LA, Feng M, Zimolzak AJ. Acute kidney injury detection using refined and physiological-feature augmented urine output. Sci Rep. 2021 Oct 1;11(1):19561. PMID: 34599217
Zimolzak AJ, Davila JA, Punugoti V, et al. Lessons Learned from an Enterprise-Wide Clinical Datathon. AMIA Annual Symposium, oral presentation. San Diego, 2021-11-02.
Ryu JH, Zimolzak AJ. Natural Language Processing of Serum Protein Electrophoresis Reports in the Veterans Affairs Health Care System. JCO Clin Cancer Inform. 2020 Aug;4:749-756. PMID: 32813561
Vassy JL, Gaziano JM, Green RC, et al. Effect of Pharmacogenetic Testing for Statin Myopathy Risk vs Usual Care on Blood Cholesterol: A Randomized Clinical Trial. JAMA Netw Open. 2020 Dec 1;3(12):e2027092. PMID: 33270123
Fillmore N, Do N, Brophy M, Zimolzak A. Interactive Machine Learning for Laboratory Data Integration. Stud Health Technol Inform. 2019 Aug 21;264:133-137. PMID: 31437900
Fillmore NR, Yellapragada SV, Ifeorah C, et al. With equal access, African American patients have superior survival compared to white patients with multiple myeloma: a VA study. Blood. 2019 Jun 13;133(24):2615-2618. PMID: 31003998
Fiore L, Ferguson RE, Brophy M, et al. Implementation of a Precision Oncology Program as an Exemplar of a Learning Health Care System in the VA. Fed Pract. 2016 Feb;33(Suppl 1):26S-30S. PMID: 30766202
Badawi O, Brennan T, Celi LA, et al. Making big data useful for health care: a summary of the inaugural mit critical data conference. JMIR Med Inform. 2014 Aug 22;2(2):e22. PMID: 25600172
Celi LA, Zimolzak AJ, Stone DJ. Dynamic clinical data mining: search engine-based decision support. JMIR Med Inform. 2014 Jun 23;2(1):e13. PMID: 25600664
Zimolzak AJ, Spettell CM, Fernandes J, et al. Early detection of poor adherers to statins: applying individualized surveillance to pay for performance. PLoS One. 2013 Nov 4;8(11):e79611. PMID: 24223977
Horstman MJ, Stewart DE, Naik AD. Improving Patients’ Post-Discharge Communication: Making Every Word Count. Circulation. 2014;130:1091-1094, PMID 25245845
Horstman MJ, Mills WL, Herman LI, Cai C, Shelton G, Qdaisat T, Berger DH, Naik AD. Patient experience with discharge instructions in post-discharge recovery: a qualitative study. BMJ Open. 2017 Feb 22;7:e014842. doi: 10.1136/bmjopen-2016-014842. PMID 28228448
Naik AD, Horstman MJ, Li LT, Paasche-Orlow MK, Campbell B, Mills WL, Herman LI, Anaya DA, Trautner DW, Berger DH. User-centered design of discharge warning tools for colorectal surgery patients. J Am Med Inform Assoc. 2017;24(5):975-980. PMID 28340218
Du RY, Shelton G, Ledet CR, Mills W, Herman L, Horstman M, Trautner B, Awad S, Berger D, Naik AD. Implementation and Feasibility of the Re-Engineered Discharge for Surgery (RED-S) Intervention: A Pilot Study. J Healthc Qual. 2020 Jun 9. doi: 10.1097/JHQ.0000000000000266. PMID: 32544139
Horstman MJ, Cowart JB, McMaster-Baxter NL, Trautner BW, Stewart DE. A human factors approach to improving electronic performance measurement of venous thromboembolism prophylaxis. Int J Qual Health Care. 2016; 28(1):59-65. PMID: 26660442
Walker M, Gay L, Raynaldo G, Von Marensdorff H, Bates JT, Friedland JA, Park JH, Kehl E, Sowers B, Bhavani S, Lan C, Bozkurt B, Stewart DE, Horstman MJ. Impact of a Resident-Centered Interprofessional Quality Improvement Intervention on Acute Care Length of Stay. J Healthc Qual. 2018 Oct 26. doi: 10.1097/JHQ. 0000000000000156. PMID: 30383558
Patel V, Stewart D, Horstman MJ. E-consults: an effective way to decrease clinic wait times in Rheumatology. BMC Rheumatol. 2020;4:54. PMID: 33073171.
Horstman MJ, Li YF, Almenoff PL, Freyberg R, Trautner BW. Denominator Doesn’t Matter: Standardizing Healthcare-Associated Infection Rates by Bed-Days and Device-Days. Infect Control Hosp Epidemiol. 2015 Jun;36(6):710-6. PMID: 25782986
Horstman MJ, Naik AD. A ‘Just Culture’ for performance measures. BMJ Qual Saf. 2015;24:486-9. PMID: 25991867
Razjouyan, Javad, et al. "A neuro-fuzzy based model for accurate estimation of the Lyapunov exponents of an unknown dynamical system." International Journal of Bifurcation and Chaos 22.03 (2012).
Razjouyan, Javad, et al. "Recurrent Map Analysis of Digital Spiral Drawing Signal to Investigate Fine Motor Movement in Multiple Sclerosis Patients and Controls." Biomedical Engineering: Applications, Basis and Communications 26.05 (2014).
Mortaza, N., Osman, N. A. A., Jamshidi, A. A., & Razjouyan, J. (2013). Influence of functional knee bracing on the isokinetic and functional tests of anterior cruciate ligament deficient patients. PloS one, 8(5), e64308.
Siahi, M., Razjouyan, J., Khayat, O., Mansouri, A. A., & Azimi, Z. (2015). A multi-class bi-level thresholding method for accurate anthropometric measurements of scanned plantar images. Signal, Image and Video Processing, 9(2), 295-304.
Razjouyan, J., Grewal, G. S., Rishel, C., Parthasarathy, S., Mohler, J., & Najafi, B. (2017). Activity monitoring and heart rate variability as indicators of fall risk: proof-of-concept for application of wearable sensors in the acute care setting. Journal of gerontological nursing.
Razjouyan, J., Naik, A. D., Horstman, M. J., Kunik, M. E., Amirmazaheri, M., Zhou, H., ... & Najafi, B. (2018). Wearable sensors and the assessment of frailty among vulnerable older adults: an observational cohort study. Sensors, 18(5), 1336.
Brown, C. J., Foley, K. T., Lowman, J. D., MacLennan, P. A., Razjouyan, J., Najafi, B., ... & Allman, R. M. (2016). Comparison of posthospitalization function and community mobility in hospital mobility program and usual care patients: a randomized clinical trial. JAMA internal medicine, 176(7), 921-927.
Razjouyan, J., Grewal, G. S., Rishel, C., Parthasarathy, S., Mohler, J., & Najafi, B. (2017). Activity monitoring and heart rate variability as indicators of fall risk: proof-of-concept for application of wearable sensors in the acute care setting. Journal of gerontological nursing.
Lindberg, C. M., Srinivasan, K., Gilligan, B., Razjouyan, J., Lee, H., Najafi, B., ... & Sternberg, E. M. (2018). Effects of office workstation type on physical activity and stress. Occupational and environmental medicine, 75(10), 689-695.
Razjouyan, J., Lee, H., Gilligan, B., Lindberg, C., Nguyen, H., Canada, K., ... & Najafi, B. (2020). Wellbuilt for wellbeing: Controlling relative humidity in the workplace matters for our health. Indoor air, 30(1), 167-179.