What Is a Scarless Thyroidectomy (Thyroid Surgery)?
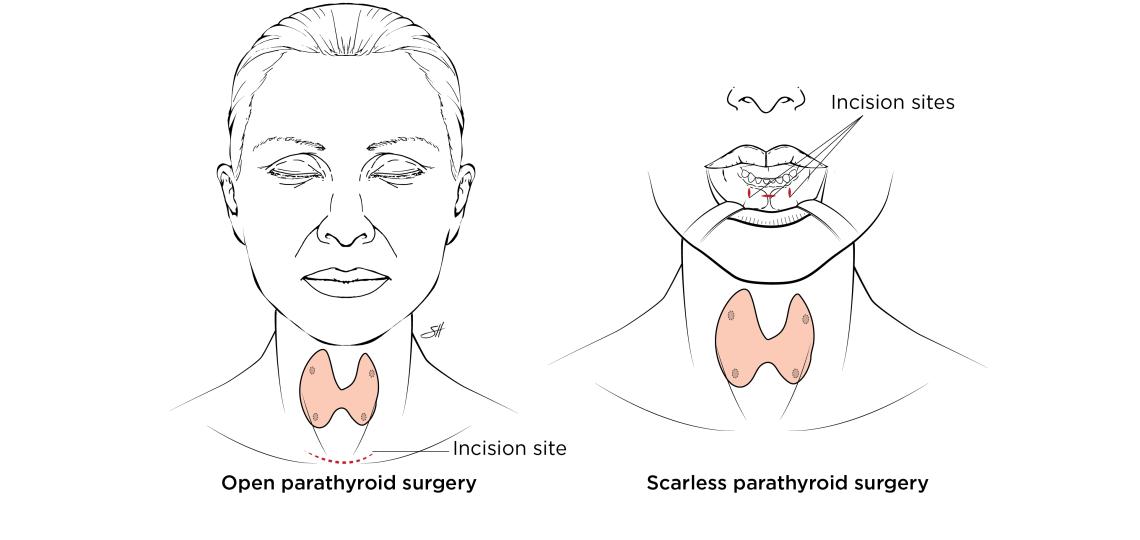
Scarless transoral thyroidectomy or transoral vestibular approach (TOVA) allows for the safe and total removal of the thyroid or parathyroid glands with absolutely no external scarring to the neck.
Of all so-called "scarless" thyroid surgeries, the transoral technique is the only one that is truly scarless. Although other types of thyroid and parathyroid techniques may not leave a scar on the neck, they do leave a scar at the alternative incision point, the armpit, hairline or nipple.
Benefits of the TOVA are two-fold: It preserves the natural appearance the neck and leaves no external reminder of the operation and provides a quick and easy recovery.
About the Scarless Transoral Vestibular Approach
The transoral vestibular approach leaves no wound on the neck because the thyroid gland is accessed through three small 3-10 mm incisions inside the lower lip. Through these incisions, small laparoscopic instruments (about the diameter of the pen) are passed under the skin and down to the thyroid or parathyroid.
Standard laparoscopic techniques are then used to remove the affected gland, which is placed inside a bag and removed through the middle incision. The incisions are closed with stitches that dissolve on their own.
Are You a Candidate for Transoral Thyroid Surgery?
Many individuals who need their thyroid or parathyroid glands removed are potential candidates for scarless thyroid surgery. Ideal candidates for this type of scarless thyroid surgery may have the following diagnoses:
- Thyroid cancer nodule less than 2 cm
- Thyroid removal for benign conditions such as goiter or Graves’ disease
- Benign thyroid nodule less than 6 cm
- Primary hyperparathyroidism
- Limited secondary or tertiary cases of hyperparathyroidism
Our multidisciplinary team thoroughly evaluates each patient to recommend the safest, most effective treatment.
What to Expect Following Surgery?
The procedure requires an overnight hospital stay. A dedicated care team closely monitors your recovery from the procedure. Patients are typically discharged the following morning.
For the first two to three days after the procedure, you can expect to have sore throat, a scratch voice and a stiff neck. There will also be some swelling and bruising on the lower lip, chin and upper neck. These symptoms should go away within seven to 10 days.
After two weeks, you may feel a sensation of firmness and tightness in the area, The tightness is a normal reaction to any surgical incision site and will go away over time.
Most patients do not require prescription-strength medication for more than two to three days after surgery, at which point an over-the-counter pain reliever like ibuprofen is sufficient.
A liquid diet is recommended for the first day after surgery, followed by soft foods on the second day. On the third day, you can return to your regular diet.
It is important to maintain good oral hygiene post-surgery, being careful not to disturb the sutures. A prescription strength mouthwash will be prescribed after surgery, which should be used for the first week post-surgery after each meal.
Is the Transoral Approach Safe and Effective?
Studies have shown that scarless thyroid removal results in similar cure rates as in conventional open thyroid surgery. As with any surgery, there are some risks associated with the procedure. However, based on current scientific literature the scarless approach seems to be as safe and effective as the traditional approach for the great majority of patients.
Fariha's Story by the Houston Chronicle
Dr. Raymon Grogan goes beyond the scope of traditional thyroid surgery on his patient Fariha. Her response “I don’t see why you wouldn’t want to do it this way,” she said. “To me, it makes so much sense. This is the way to go for sure.”

Cindy's Story
"Personally, I just did not want the always present reminder that I'd had cancer. Call me vain, but I also was concerned about the appearance of the scars that I had seen on some family members that had their thyroid removed. Some weren't as bad as others, but I did not want to feel self-conscious or have to wear high-necked shirts during the summer to camouflage the scar." - Cindy