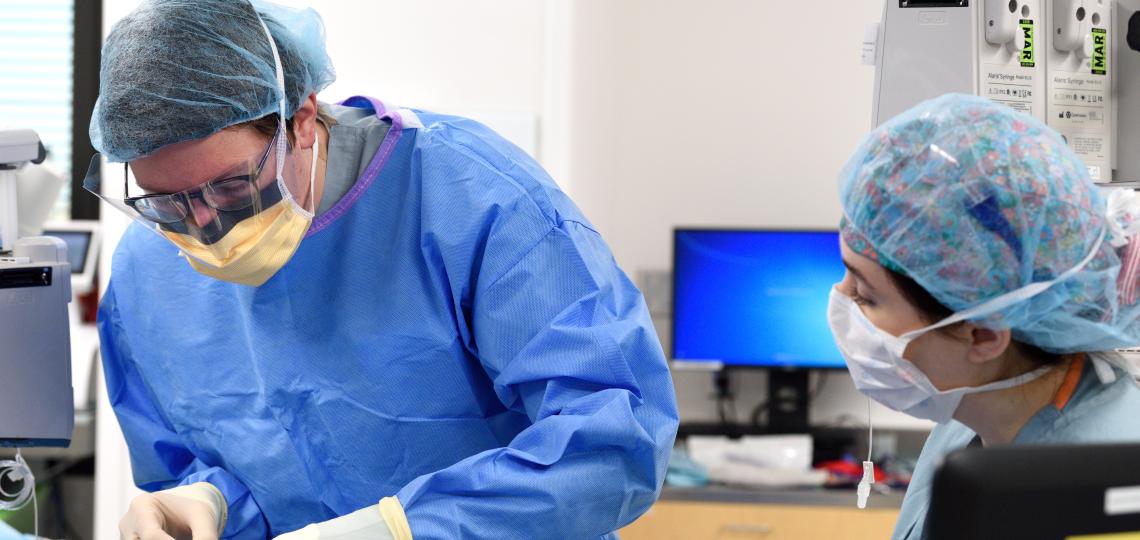
Rotations
Core Rotations
Fellows rotate through the CVOR, cardiac catheterization laboratories and diagnostic imaging (MRI, CT, IR) one week at a time. For example, if assigned to the CVOR, then this would be your location for the week. There is flexibility to shift out of locations based on case needs and learning opportunities. The ratio of CVOR: cath lab approximates 3:1.
Electives: 4 weeks
Elective options are tailored to your interests including echocardiography, international experiences (Bolivia and Jamaica through our faculty who have worked at these sites over the years), catheterization (with interventional cardiology), transfusion medicine (reviewing management of patients on ECMO and those with other clotting/bleeding derangements), perfusion (bypass management), research, etc. In recent years fellows have also rotated at our sister institution, the Texas Heart Institute, for additional experience in managing traditional adult cardiac surgery and catheter-based interventions.
ICU: 4 weeks
Divided into 1 week blocks with a focus on pre-operative and post-operative management in the neonatal and heart failure units. Fellows are present as observers with no front-line responsibilities.
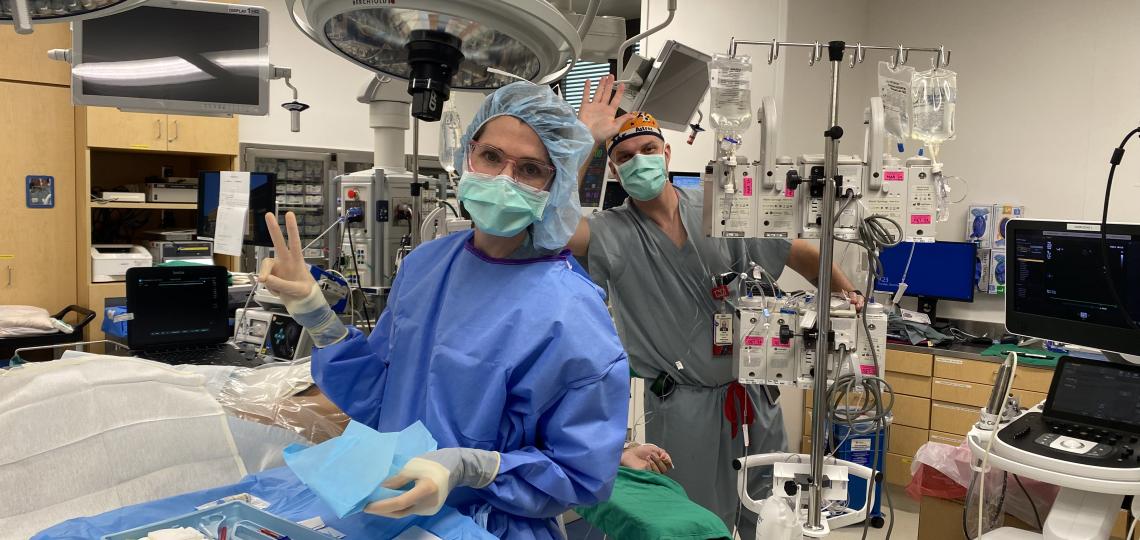
Call
The cardiovascular anesthesiology fellow(s) will be in the call pool with general pediatric anesthesia fellows, rotating CA3 residents, adult cardiac anesthesia fellows and cardiac CRNAs. Our CV fellows average 4-5 calls/month.
Typically, the call fellow is assigned to what is predicted to be the longest case of the day. On weekdays, in-house call ends following the completion of the last case. Afterwards, the fellow is on pager call from home until 7 a.m. the following day. On weekends, the call is a pager call from home and covers a 24-hour period. The day following call is ALWAYS a true post-call day with no clinical responsibilities, no matter what time cases finish the day before.