We believe that our clinical volume and complexity are one of the greatest strengths of our program. Reflecting this volume are our anesthetizing locations, which include:
- 4 cardiovascular operating rooms
- 3 cardiac catheterization labs
- 1 electrophysiology lab
- A procedure room suite
- CT
- MRI
- Interventional radiology
At all of these sites, our fellows are paired 1:1 with an attending anesthesiologist, thereby increasing the fellows’ procedural experience as well as fellow-level directed learning. In our operating rooms, fellows routinely place the necessary central and arterial lines.
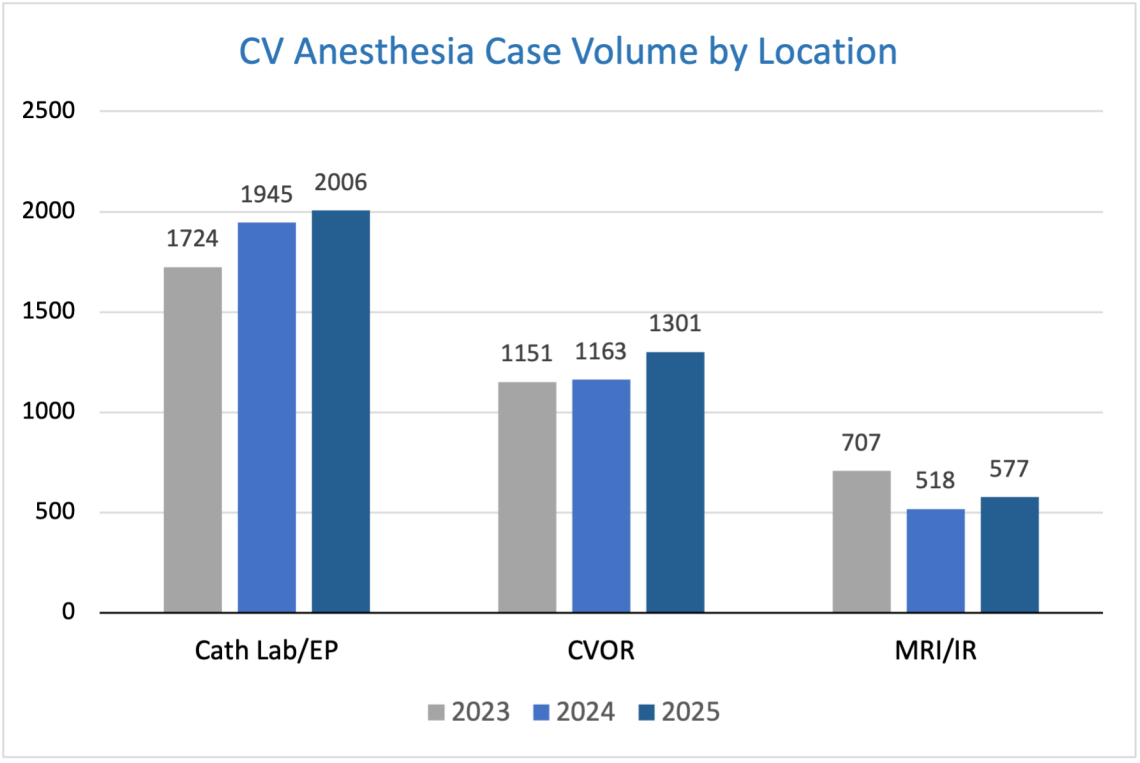
Below are data demonstrating our Heart Center case volume as well as fellows’ case numbers over recent years. The end-result of our clinical experience is that our fellows are well-prepared to manage any patient presenting for any procedure.
| Case Type | Total |
|---|---|
| Stage 1 Palliation (Norwood) | 54 |
| Bidirectional Cavopulmonary Anastomosis (BDG) | 89 |
| Fontan | 120 |
| Arterial switch (dTGA and dTGA/VSD) | 48 |
| Truncus arteriosus | 17 |
| Tetralogy of Fallot | 102 |
| Complete atrioventricular septal defect | 50 |
| Coarctation of the aorta, off-bypass | 73 |
| Heart transplant | 120 |
| Lung transplant | 28 |
| VAD implant | 86 |
| Adult congenital | 421 |
Procedure | Average | Range |
|---|---|---|
| Bypass cases, fellow as sole trainee | 107 | 95-136 |
| Stage 1 Palliation (Norwood) | 7 | 3-10 |
| Bidirectional Cavopulmonary Anastomosis (BDG) | 8 | 5-10 |
| Fontan | 7 | 3-10 |
| Arterial switch | 6 | 5-9 |
| Other neonatal surgical procedures | 14 | 4-26 |
| Coarctation of the aorta | 4 | 3-5 |
| Cardiac or lung transplant | 7 | 6-10 |
| Placement of circulatory assist device | 14 | 10-19 |
| Catheterization/EP procedures | 73 | 30-102 |
| Central venous line placement | 103 | 90-112 |
| Arterial line placement | 113 | 102-143 |
| Neonatal anesthetics, total | 49 | 28-75 |
| Adult congenital anesthetics, total | 31 | 20-48 |