The Center for Cardiac Engineering & Regenerative Therapeutics in the Department of Surgery is pioneering innovative gene therapies designed to repair and restore damaged heart tissue. Our research focuses on a combination of three cutting-edge approaches:
- Direct cardiac reprogramming
- Induction of the cell cycle in cardiomyocytes
- Induce angiogenesis
Through extensive studies, we aim to optimize these strategies and unlock the full potential of cardiac regeneration. Preclinical animal models have demonstrated promising results, including improved heart function and tissue repair following gene delivery.
We are actively exploring safe and efficient delivery methods, such as viral and non-viral vectors, to introduce therapeutic genes into the heart. Our team is also investigating:
- The most effective gene combinations
- The optimal timing for delivery
- The molecular mechanisms driving regeneration
Our ultimate goal is to develop targeted, personalized therapies for patients with heart disease, transforming the future of cardiac care.
Publications
In the News
- BCM to lead cardiac innovation AI-driven drug safety project
- Breakthrough cardiac regeneration research offers hope for the treatment of ischemic heart failure
- Not too late to repair: gene therapy improves advanced heart failure in animal model
- Jessica Miller Receives SPS Technological Innovation Publication Award
- Study finds elimination of p63 gene could convert scar tissue into muscle tissue in the heart
- Dr. Todd Rosengart Awarded NIH-NHLBI Grant for Cardiac Cellular Reprogramming
- Innovative approach brings cell-reprograming therapy for heart failure closer to reality
- Dr. Rosengart named National Academy of Inventors Fellow
Cardiac regeneration gene therapy involves the use of specific genes to stimulate the regeneration of damaged heart tissue.
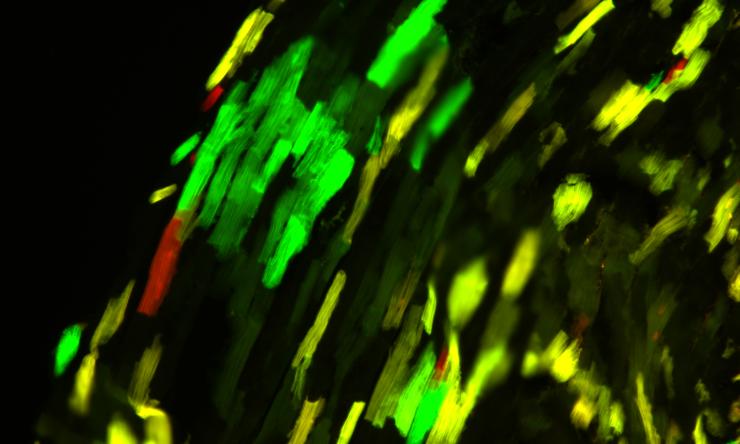
The induction of the cell cycle in cardiomyocytes involves the activation of specific genes that are responsible for regulating cell division and growth.
Heart slice culture is a technique that allows researchers to study the structural and functional properties of heart tissue in a controlled laboratory setting.
