Michael E. DeBakey, M.D.
Early Years
Michael E. DeBakey, M.D., born Sept. 7, 1908, in Lake Charles, La., was the first of five children of Lebanese immigrants Shaker Morris and Raheehja DeBakey. Valedictorian of his high school class, he pursued a college education at Tulane University.
At Tulane, he earned enough credits by the end of his second year to enter medical school. He combined his final undergraduate courses with medical studies. As a result, he received his B.S. in 1930, his M.D. in 1932, and an M.S. in 1935. During his final year in medical school, he created the roller pump. Two decades later, it became a crucial component of the heart-lung machine that paved the way for open-heart surgery.
Following an internship at Charity Hospital in New Orleans, he continued his studies in Strasbourg, France, and Heidelberg, Germany. Returning to the United States in 1937, he joined Tulane's faculty. At the beginning of World War II, he volunteered to serve in the armed forces. As Colonel Michael DeBakey, he served on the Army Surgeon General's staff. During this time, he published a number of papers about treating chest wounds and vascular injuries in injured military personnel. His work led to the development of mobile army surgical hospitals or MASH units. In addition, he helped establish the system of treating military personnel returning from the war, a concept that evolved into the Veterans Affairs Medical Center System, now the Department of Veterans Affairs. For his service, he received the U.S. Army Legion of Merit Award.
Educator
In 1948, Dr. Michael E. DeBakey accepted the chairship of the Department of Surgery at Baylor College of Medicine, then newly established in Houston. He helped establish the school's residency programs, starting with surgery.
In 1969, he was named the College's president. In his 10-year tenure in that office, he propelled Baylor toward national and international acclaim as one of the best medical schools in the United States.
One of his proudest educational achievements was the establishment of the Michael E. DeBakey High School for Health Professions, a joint project of Baylor and the Houston Independent School District.
The school enabled students, many of them members of underrepresented minorities, to obtain the basic education they needed to do well as undergraduates and eventually enter medical school.
In 1978, he assumed the post of chancellor, in which he served until 1996, when he became chancellor emeritus. A number of buildings, organizations and awards pay tribute to his dedication to the College.
During his career, DeBakey wrote more than 1,400 articles, chapters and books including two New York Times best-sellers: The Living Heart and The New Living Heart Diet. Other popular books he co-authored include The Living Heart Brand Name Shopper's Guide, The Living Heart Guide to Eating Out and The New Living Heart.
Surgeon
Best known for his trailblazing efforts in the treatment of cardiovascular diseases, Dr. Michael E. DeBakey was the first to perform successful excision and graft replacement of aneurysms of the thoracic aorta and obstructive lesions of the major arteries. A pioneer in the development of an artificial heart, he was the first to use a partial artificial heart -- a left ventricular bypass pump, successfully.
In 1953, DeBakey performed the first successful carotid endarterectomy, thereby establishing the field of surgery for strokes. In 1963, he received the first federally funded grant to establish a program for the development of artificial heart pumps, a project on which he had long labored. In the 1950s, he also developed the first Dacron grafts designed to replace areas of arteries weakened by aneurysms. In 1964, DeBakey and associates performed the first successful aortocoronary-artery bypass with autogenous vein graft. In 1966, he was the first to successfully implant a left ventricular assist device, which helped failing hearts pump blood. In 1968, he led a team of surgeons in a historic multiple-transplantation procedure in which the heart, kidneys, and one lung of a donor were transplanted to four recipients.
He and colleagues developed the DeBakey Ventricular Assist Device, which he believed could help a failing heart pump blood. He believed that two working together could function as a total heart replacement.
A prolific physician and teacher, DeBakey performed more than 60,000 cardiovascular procedures and trained more than 1,000 surgeons who now practice throughout the world. The Michael E. DeBakey International Cardiovascular Surgical Society was founded Jan. 20, 1977, in honor of his dedication to teaching. Subsequently renamed the Michael E. DeBakey International Surgical Society, this organization perpetuates DeBakey's vision through scholarship, training and recognition.
Medical Statesman
Since World War II, DeBakey served as an advisor to most American presidents. In 1949, as a member of the Task Force on Medical Services of the Hoover Commission on Organization of the Executive Branch, he led the movement to establish the National Library of Medicine, which now contains more than 6.2 million books, journals, technical reports, manuscripts, microfilms, and pictorial and audiovisual materials. He was also chair of the President's Commission on Heart Disease, Cancer and Stroke.
DeBakey did not limit his work as a medical statesman to the United States. He helped establish cardiovascular surgery programs and even health-care systems in a number of countries, including Germany, China, Italy, Australia, Japan, Saudi Arabia, Egypt and Spain, as well as nations in Central and South America.
He received approximately 50 honorary degrees from colleges and universities and more than 200 awards from educational institutions, civic organizations and governments worldwide. Among his major awards are the Medal of Freedom, the highest honor the President of the United States bestows upon a civilian, the Lasker Award (the American equivalent of the Nobel Prize) and the Congressional Gold Medal.
Timeline of Contributions to Medicine

Explore a timeline of Dr. Michael E. DeBakey's contributions to medicine through his lifetime.
1953
DeBakey performed the first successful removal of a blockage, or lesion, of the carotid artery, the main artery of the neck that supplies blood to the brain. During this procedure, called an endarterectomy, the surgeon slits the artery open, peels away the lesion from the artery wall and then closes the incision by sewing the remaining undamaged walls. This accomplishment showed that a major cause of strokes could be treated effectively.
1954
He followed with the first successful resection and graft replacement of an aneurysm in the downward section of the aortic arch, which curves like a cane handle over the top of the heart. He also did the first successful resection of an aneurysm in the muscle layer of the aorta, and the first successful resection and graft replacement of an aneurysm of the upper part of the aorta.
1955
DeBakey was the first to do a successful resection of an aneurysm of the portion of the aorta between the chest and abdomen. This procedure was performed with a graft replacement of the arteries leading from the aorta to the liver, spleen, stomach, gastrointestinal tract and kidneys.
1958
To counteract narrowing of an artery caused by an endarterectomy, DeBakey developed the first patch-graft angioplasty. This procedure involved patching the slit in the artery from an endarterectomy with a Dacron or vein graft. The patch widened the artery so that when it is closed, the channel of the artery returned to normal size.
1960s
1963
DeBakey developed the concept behind the coronary bypass by noting that in many forms of arterial disease, the portions above and below a diseased or blocked segment of artery were normal. Therefore, the damaged portion could be bypassed to restore blood flow and prevent a fatal heart attack. A year later, he performed the first successful coronary bypass using the large vein in the leg to bypass the blocked or damaged area between the aorta and coronary arteries.
1965
DeBakey pioneered the field of telemedicine with the first demonstration of open-heart surgery to be transmitted overseas by satellite. A medical staff at a hospital and university in Geneva were able to view an aortic-valve replacement being performed at The Methodist Hospital in Houston.
1966
He was the first to successfully use the left ventricular bypass pump. This device took oxygenated blood from the left atrium, one of the chambers of the heart that receives blood from the lungs and body, and pumped it back into circulation by a connection to the aorta or a major artery.
1968-70
DeBakey performed 12 heart transplants. The program was discontinued in the early 1970s because of problems with organ rejection.
1970s
DeBakey continued testing artificial-heart models to sustain the lives of calves, a research program he began in the 1960s. He also studied ways to eliminate the risk of stroke and the cumbersome nature of current artificial heart devices.
1975
DeBakey received a federal grant to establish the first National Heart and Blood Vessel Research and Demonstration Center. He had previously recommended development of highly specialized centers in different parts of the nation to treat wounded veterans, and then applied the center concept to civilian medicine by establishing the Cardiovascular Research and Training Center at The Methodist Hospital in Houston. That center's successful multidisciplinary approach to cardiovascular research and therapy was continued at the federally-funded National Heart and Blood Vessel Research and Demonstration Center at BCM.
1980s
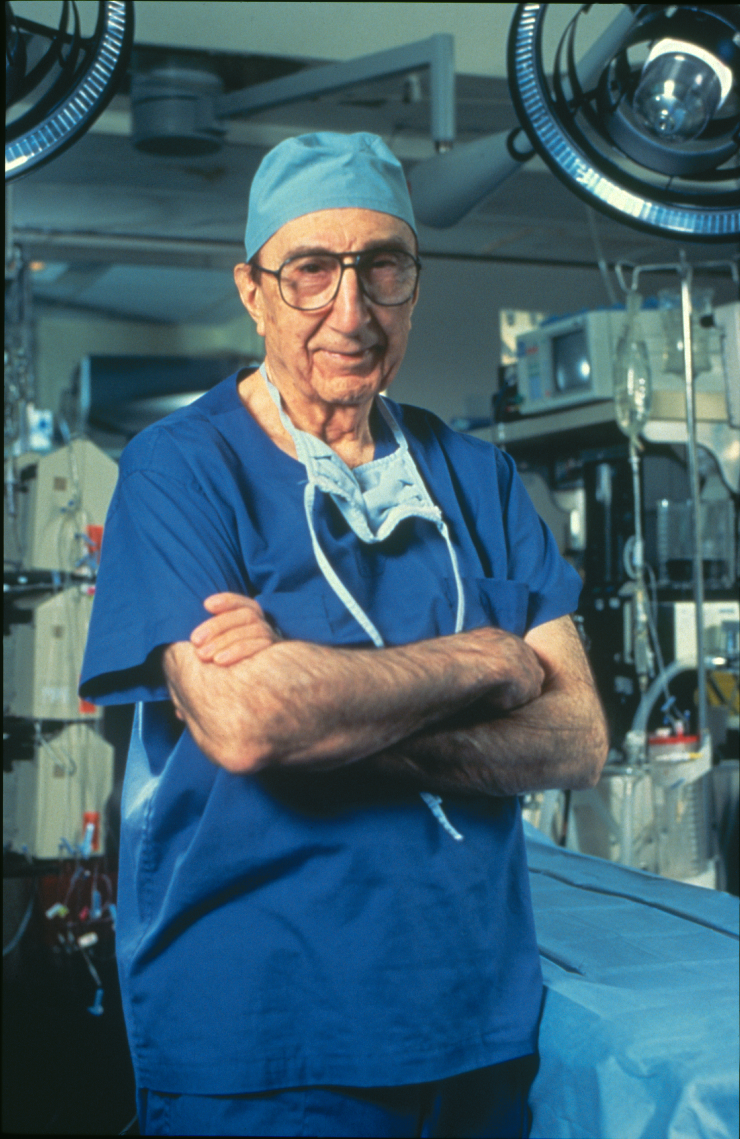
1983
DeBakey and colleagues reported that evidence of cytomegalovirus (CMV), a common virus infecting a high percentage of people without causing symptoms, was present in the walls of 11 patients with atherosclerosis, or hardening of the arteries. CMV, which causes cells to multiply, often becomes dormant in the body for years after infection. The study suggested that early in life, CMV might initiate the lesions that later cause atherosclerosis.
1984
Encouraged by the development of cyclosporine to prevent organ rejection, DeBakey resumed heart transplantation.
1987
A second report on CMV by DeBakey and colleagues found that heart-disease patients have higher-than-normal levels of antibodies to CMV. The report supported their earlier finding that CMV might play a major role in the development of atherosclerosis.
DeBakey also reported on two other studies in 1987. One study found that cholesterol levels in 15,000 patients were unrelated to how quickly blockage of major arteries progressed. In another 1,400 patients, all of whom had undergone coronary-artery bypass surgery, he found that patients with normal or below-normal cholesterol levels were just as prone to have their replacement arteries become clogged again. While a high-fat diet, smoking and high blood pressure place a person at a higher risk of developing heart disease, these studies imply that they do not in themselves cause atherosclerosis.
1990s
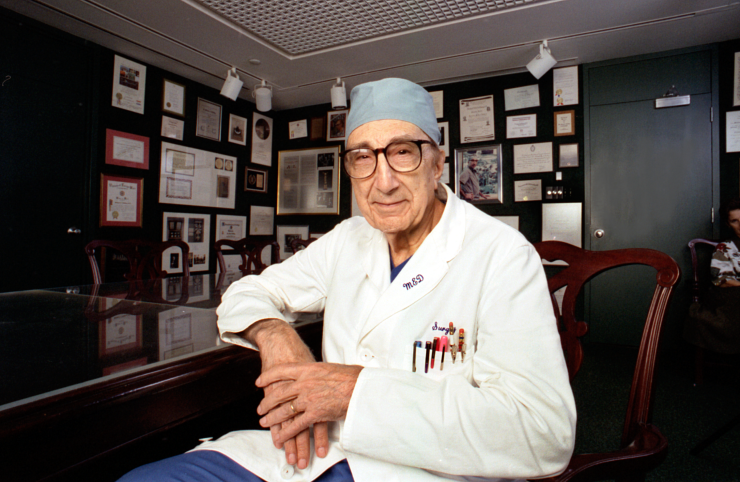
DeBakey continued to participate in telemedicine conferences and analyze statistics on the causes of atherosclerosis.
1996
He served as a consultant to the medical team that performed quintuple-coronary- bypass surgery on Russian President Boris Yeltsin. DeBakey was consulted again in 1998 at Yeltsin's request by a Russian delegation seeking advice on establishing a high-tech surgical center in Russia.
1998
Working with NASA engineers, DeBakey and colleagues refined the left ventricular heart-assist pump, known as the VAD. European clinical trials of the DeBakey Ventricular Assist Device in humans began.
Awards and Recognitions
Congressional Gold Medal (2008)
Lasker Clinical Medical Research Award renamed as the Lasker DeBakey Clinical Medical Research Award (2007)
History Making Texan Award, the Texas State History Museum Foundation (2006)
The Association of American Medical Colleges David E. Rogers Award (2004)
Veterans Affairs Medical Center named in DeBakey's honor (2004)
American Heart Association Lifetime Achievement Award (2003)
Lomonosov Large Gold Medal, Russian Academy of Sciences (2003)
The Ben Taub Humanitarian Award (2003)
Medal of Merit, International Academy of Cardiovascular Sciences (2002)
MUSC "Lindbergh-Carrel Prize" (2002)
International Academy of Cardiovascular Sciences Medal for Distinguished Achievements in Cardiovascular Sciences (2002)
NASA Invention of the Year Award (2001)
Houston Hall of Fame (2001)
Villanova University Mendel Medal Award (2001)
Library of Congress Bicentennial Living Legend Award (2000)
American Philosophical Society Jonathan Rhoads Medal (2000)
American Medical Association Virtual Mentor Award (2000)
1990s
Lifetime Achievement Award for Science and Technology from Children Uniting Nations (1999)
Texas Senate and House of Representatives, Adoption of Resolutions honoring Dr. DeBakey for 50 years of medical practice in Texas (1999)
Russian Academy of Sciences Foreign Member (1999)
John P. McGovern Compleat Physician Award (1999)
Research!America's Lifetime Achievement Award (1998)
Karolinska Institute's Honorary Degree of Doctor of Medicine and the title "Foreign Adjunct Professor" (1997)
Russian Military Medical Academy, Boris Petrovsky International Surgeons Award and First Laureate of the Boris Petrovsky Gold Medal (1997)
Premio Giuseppe Corradi Award for Surgery and Scientific Research (1997)
Common Wealth Award, Sigma Xi
Health Care Hall of Fame (1996)
Women's International Center Samaritan Living Legacy Award (1994)
Giovanni Lorenzini Foundation Prize for the Advancement of Biomedical Science (1994)
Texas Society for Biomedical Research Distinguished Service Award (1994)
American Heart Association Lifetime Achievement Award (1994)
Foundation for Biomedical Research Lifetime Achievement Award (1991)
American College of Healthcare Executives Honorary Fellow (1990)
American Legion Distinguished Service Award (1990)
The Michael DeBakey Medal, American Society of Mechanical Engineers (1990)
William Procter Prize for Scientific Achievement, Sigma Xi
1980s
The Michael DeBakey Medal, American Society of Mechanical Engineers (1989)
Association of American Medical Colleges Special Recognition Award (1988)
Academy of Surgical Research Markowitz Award (1988)
National Medal of Science (1987)
Theodore E. Cummings Memorial Prize for Outstanding Contributions in Cardiovascular Disease (1987)
First President of the Association of International Vascular Surgeons (1983)
Institute of Medicine of the National Academy of Sciences (1982)
Chair of the Board of Governors, Foundation for Biomedical Research (1981)
American Surgical Association Distinguished Service Award (1981)
Veterans of Foreign Wars Commander-in-Chief's Medal and Citation (1980)
Merit Order of the Republic of Egypt, First Class (1980)
Independence of Jordan Medal (1980)
1970s
Texas Scientist of the Year, Texas Academy of Science (1979)
Michael E. DeBakey International Cardiovascular Surgical Society formed by DeBakey's former students; name was later changed to the Michael E. DeBakey International Surgical Society to include more of his surgical residents and trainees (1976)
U.S.S.R. Academy of Science 50th Anniversary Jubilee Medal (1973)
1960s
Presidential Medal of Freedom with Distinction (1969)
Eleanor Roosevelt Humanities Award (1969)
American Heart Association Gold Heart Award (1968)
Prix International Dag Hammarskjold Great Collar with Golden Medal (1967)
American Medical Association Billings Gold Medal Exhibit Award (1967)
Medical World News Doctor of the Year (1965)
Albert Lasker Award for Clinical Medical Research (1963)
1950s
American Medical Association Distinguished Service Award (1959)
Leriche Award (1959)
International Society of Surgery Distinguished Service Award (1958)
American Medical Association Hektoen Gold Medal Award (1954 and 1970)
Rudolph Matas Award in Vascular Surgery (1954)
1940s
Task Force on Medical Services of the Hoover Commission on Organization of the Executive Branch of the Government (1949)
Legion of Merit, United States Army (1945)
Additional Honors
Tulane Medical Alumni Association
International Health and Medical Film Festival
International College of Angiology
Encyclopedia Britannica
Lifetime Achievement Awards from the Academy of Medical Films
Selected Awards and Honors from Baylor College of Medicine
Michael E. DeBakey, M.D., Library and Museum (2006)
BCM Alumni Association Lifetime Achievement Award (2006)
Distinguished Service Award (1998)
Award, photo exhibit, scientific symposium and black-tie gala honoring DeBakey's 50th anniversary at Baylor College of Medicine (1998)
Honorary Degree: Doctor of Letters in Medicine (1996)
Chancellor Emeritus (1996)
Michael E. DeBakey, M.D., Excellence in Research Awards, established in his honor with funds from the DeBakey Medical Foundation and presented annually to Baylor faculty whose research has made significant advances in basic or clinical science (1995)
President's Distinguished Service Award (1992)
DeBakey-Bard Chair in Surgery, established in his honor (1990)
Trustees Medallion (1988)
The DeBakey Heart Center established by Baylor College of Medicine and The Methodist Hospital, with DeBakey serving as director (1985)
Michael E. DeBakey Lectureship (1982)
Olga Keith Wiess Chair of Surgery (1981)
Michael E. DeBakey Center for Biomedical Education and Research (1980)
Chancellor (1978-96)
Faculty/Staff Recognition Award (1977, 1979, 1984, 1989, 1994)
Michael E. DeBakey Professorship of Pharmacology established in his honor; in 1995 became the Michael E. DeBakey, M.D., Chair of Pharmacology (1977)
DeBakey Day, Dec. 13, honoring 27 years of service (1976)
Baylor Alumni Distinguished Faculty Award (1973)
DeBakey Scholar Program established in his honor to provide funds to a medical student who has demonstrated outstanding scholarship throughout the basic and clinical sciences (1972)
President (1969-79)
Vice President for Medical Affairs and Chief Executive Officer (1968-69)
Distinguished Service Professor (1968)
Chair of Surgery (1948-93)