Foix Alajouanine Syndrome
Patient #3 presented with a syndrome that is extremely rare and difficult to treat. The patient had evidence of spinal cord compromise at a L3-S1 level. Spine xrays and a routine myelogram failed to define the problem. However, a MRI and CT post myelogram did demonstrate thoracolumbar enlargement. A spinal select angiogram was required to define the presence of a spinal epidural arteriovenous fistula at the level of S1.
Arterial embolization by selective catheterization of the right iliac artery was performed. Frontal and oblique projections revealed the spinal epidural fistula at the level of approximately S1, fed by a branch of the lateral sacral artery. A draining vein extended intradurally to the level of the conus. A 5 french guiding catheter was in place. Through this catheter a tracker 10 catheter was maneuvered into the feeding artery itself. Using road mapping technique, and under fluoroscopic control, liquid adhesive agent was instilled into the fistula with extension of adhesive agent into the draining vein for full, complete obliteration of the fistula. A post treatment internal iliac arteriogram demonstrated complete obliteration of the fistula without residual malformation. Post treatment right common iliac arteriogram was normal in appearance without identification of any vascularity to the level of the fistula.
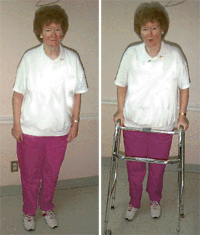
Following embolization, the patient was able to stand and use a walker for short distances
The patient did well throughout her hospitalization and regained some motor function in her lower extremities (iliopsoas 3/5, quadriceps and hamstrings 3/5, tibialis anterior and gastrocnemius 3/5). Prior to embolization she was wheelchair bound. Three days following embolization, she was able to stand and use a walker for short distances. The major improvement came from decreasing the venous congestion and compression of the spinal cord. She still had incontinence and absent sensation in the perianal area. Transfer to a rehabilitation center was necessary for continued physical therapy.
"Foix-Alajouanine Syndrome" (FAS) or "Subacute necrotic myelopathy" was originally described by Foix and Alajouanine in 1926. Two patients were reported having a progressive disorder involving the spinal cord which compromised blood supply, resulting in varying degrees of paraplegia. The other names which have been used for this condition include "angiohypertrophic necrotizing myelitis", "angiodysgenetic myelomalacia", and "angiodysgenetic necrotizing myelopathy". The syndrome of Foix-Alajouanine is not a separate disease per se but represents a specific type of chronic radiculomyelopathy, the underlying cause of which is most commonly an intradural arteriovenous malformation.
FAS is a chronic radiculomyelopathy and the underlying cause is most commonly an intradural AVM. Spinal AVM's are of four main types:
Symptoms are thought to be produced when there is vascular compromise and infarction of spinal cord tissue. Factors important for the pathogenesis of the radiculomyelopathy seen with the AVM's include:
All or some of these factors are responsible.
Macroscopically, the spinal cord is covered by coiled and convoluted vessels, more on the dorsal than on the ventral surface. The cord tends to be shrunken, cystic in parts and discolored. Microscopically, in addition to considerable thickening and redundancy of vessels in the subarachnoid space and along the intradural parts of the spinal roots, there is also extensive demyelination and necrosis of the cord. This may be patchy of may affect the cord transversely. There is also striking increase and proliferation of blood vessels both within and outside the necrotic areas.
The majority of affected patients are males older than 50 years of age. They may present with symptoms consistent with a myelopathy which may be due to the above mentioned reasons. About half of the patients have an acute onset of pain and dysesthesia or may complain of intermittent sciatica. Patients may have a full blown myelopathic picture or may have transient weakness and sensory disturbances followed by progressive radiculospinal symptoms. There may also be bowel or bladder incontinence and impotence.
Diagnosis is established by the history of acute and intermittent symptoms described above and the following imaging studies:
The prognosis of this disease depends on the underlying etiology for the symptoms, type of AVM, recognition of the clinical syndrome, and availability of specialized techniques. Venous congestion may block the draining veins and compromise spinal cord function. Thus embolization of the arterial feeders may potentially decrease the blood supply, decrease venous congestion, and improve spinal cord function. This has been shown to be of major benefit in limited trials. Supportive measures for spasticity and bladder and bowel dysfunction may also be of value.
Email comments: