PLAIN RADIOGRAPHIC DIAGNOSIS OF CONGENITAL HEART DISEASE |
Contents | Previous Condition | Next Condition
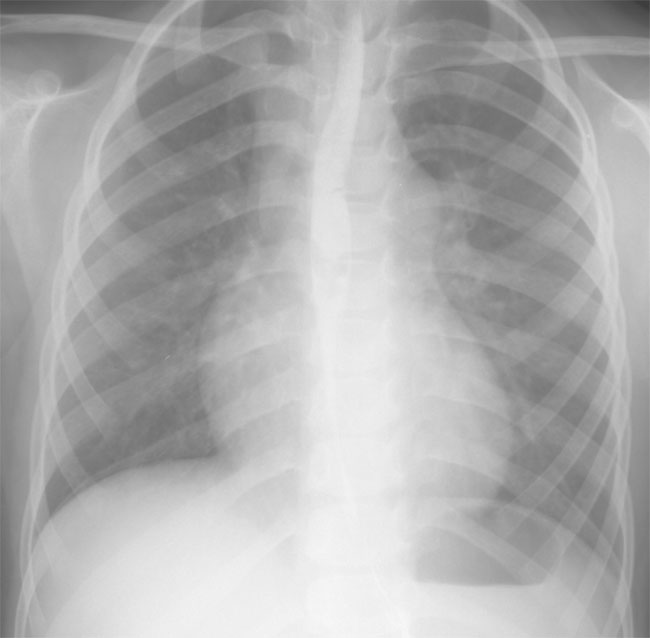
A. PA chest film demonstrates normal heart size. The pulmonary artery is abnormally convex with normal branch pulmonary arteries. The aortic arch is left-sided.

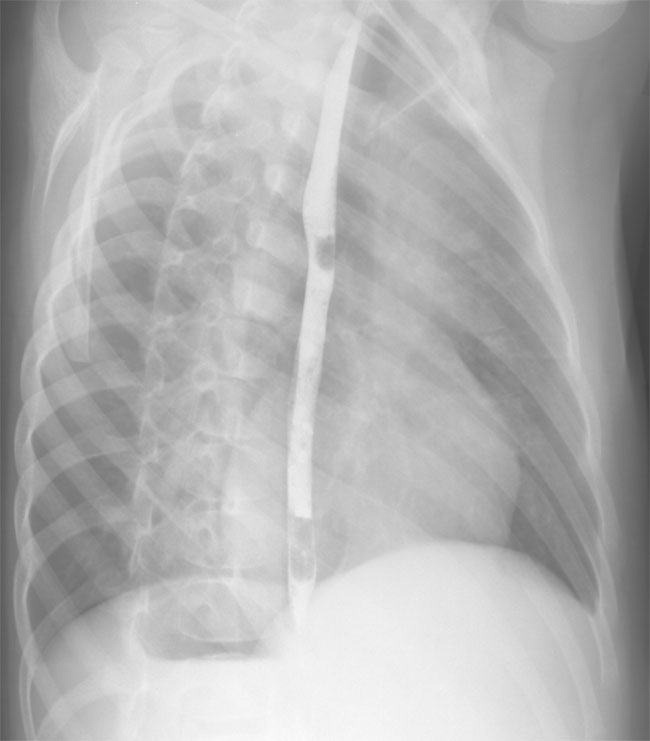
B. Right posterior oblique view demonstrates right ventricular dilation with increased convexity of the anterior chamber.
Pulmonary stenosis was originally described by Morgagni and may be classified as valvular, infundibular or supravalvular. Some form of pulmonary stenosis occurs in up to 20-30% of patients with congenital heart disease. One study from Toronto Children’s reported pulmonary stenosis in 9.9% of all congenital heart lesions.
Anatomy: There are six types of pulmonary valve in association with stenosis including, domed, unicommissural, bicuspid, tricuspid, hypoplastic annulus, and dysplastic. Dysplastic pulmonary valvular stenosis is typical of that seen in Noonan’s syndrome and less common conditions including LEOPARD and Watson syndromes.
Classification:
Physical findings: These obviously depend on severity of right ventricular outflow tract obstruction. In mild stenosis, the jugular venous pulse, pulses and precordium are normal. There is often a systolic ejection click secondary to doming of the valve, which moves closer to the first heart sound with increasing severity of the stenosis. The second heart sound is normally split and becomes increasingly split with increasing severity of stenosis. The pulmonary component of the second heart sound decreases with increasing severity. The murmur is typically an ejection systolic murmur located at the left upper sternal edge, which radiates to the back. The murmur duration and harshness increases with increasing obstruction and may even disappear with near total obstruction. The murmur increases in intensity following amyl nitrate inhalation, which is the opposite of aortic valve stenosis. Co-existent pulmonary regurgitation should be listened for in addition to a diastolic rumble of an associated atrial septal defect. Severe stenosis may be accompanied by elevated A waves in the JVP, a tapping apex beat, a right ventricular heave, a thrill in the left second intercostal space and a harsh long systolic murmur. The ejection click occurs close to the first heart sound and the second heart sound may be soft. There may be evidence of right heart failure.
ECG: There is almost always abnormality in severe PS, with right axis deviation and right ventricular hypertrophy. There may also be right atrial enlargement and T wave changes
Treatment: Transcatheter pulmonary balloon valvuloplasty in children was first performed by Kan in the early 80s. Balloon valvuloplasty is generally advocated if the gradient is greater than 40-50mmHg. Surgical valvectomy is rarely required in isolated pulmonary valve stenosis indicating the success of valvuloplasty.