Present Illness: A 53 year old, left-handed Hispanic gentleman was evaluated by the Neurology Service at the VA Medical Center for progressive memory problems and difficulty executing complex tasks. About five years ago, his family began to notice that he was having trouble counting merchandise correctly and could not handle money well. His problems have slowly but progressively worsened. He became no longer able to do the family finances, and while he was able to drive, he got lost easily. His family noted that he could no longer write words nor dial a telephone. While he worked for several years in auto repair business, he became unable do basic repairs, including simply putting a lock together. He was no longer able to read a newspaper because "the layout was confusing and he tried to read it like a book." He had moderate difficulty reading globally because his "eyes jump around from line to line." However, despite these cognitive complaints, he did not need verbal reminders. He remembered to take his medicines without the aid of a pill box. He had no difficulty feeding, dressing, or bathing himself. He denied feeling depressed. He and his family denied hallucinations, notable variability in his cognitive symptoms, abnormal movements, nor urinary incontinence. He was diagnosed with "multiple sclerosis" at an outside institution three years ago based on his brain MRI findings, but was not started on medication at that time. He has had no episodes of transient or permanent vision loss, weakness, or numbness.
Past Medical History: Hypothyroidism, hypercholesterolemia, and migraines. A concurrent diagnosis of "multiple sclerosis," per patient.
Medications: Aspirin 81 mg daily, levothyroxine 0.05 mg daily, simvastatin 80 mg daily.
Family History: Maternal uncle with Alzheimer's disease. Mother with colon cancer.
Social History: He was married, living with his family. He previously worked as a traveling salesman. He also earlier worked in the auto repair business. His family reported that he has been "always a little slow" cognitively. He stopped working secondary to cognitive problems. He formerly drank alcohol heavily, but has abstained for the last ten years. He admitted remote smoking history, but denied abuse of illicit drugs. He denied significant travel history other than to Mexico.
Review of Systems: No fevers, chills, night sweats, sick contacts, weight loss. No chest pain, shortness of breath, nausea, vomiting, diarrhea, constipation, skin rashes, heat or cold intolerance, hair or skin changes. He felt healthy other than the above complaints.
General: Pleasant and cooperative, middle-aged gentleman in no acute distress.
Vital Signs: Temperature 97.1 F, pulse 72/min, respiratory rate 20/min, blood pressure 123/75 mm Hg.
HEENT: Normocephalic, without evidence of trauma. Sclerae and conjunctivae clear. Nasopharynx and oropharynx clear. Mucous membranes moist.
Neck: Supple, no lymphadenopathy, no jugular venous distension, no bruits.
Chest: Clear to auscultation.
Cardiovascular: Regular rate and rhythm, normal S1 and S2, no S3, no murmurs.
Cerebellar: Intact finger-to-nose, heel-to-shin, and rapid alternating movements without difficulty. No bradykinesia.
Gait: Steady, normal stance and arm swing. No difficulty with toe, heel, or tandem gait.
Abdomen: Soft, nontender, nondistended, no organomegaly.
Extremities: No clubbing, cyanosis or edema.
Skin: No rashes.
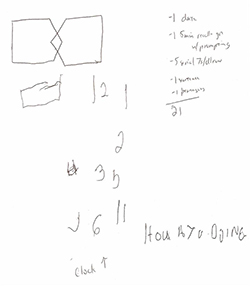
Written sample
Mental Status: Speech fluent with normal naming, normal repetition, but some impaired comprehension. MMSE = 21/30 (-1 for day of the week, -1 for 5 min recall, -5 on serial 7s, -1 for drawing of pentagons, -1 for his written sentence). He was unable to draw a clock and
Cranial Nerves: Pupils were equally round and reactive to light and accommodation. Full voluntary horizontal and vertical eye movements, but poor smooth pursuit. Voluntary saccades were impaired with need for multiple adjustments to the target. Impaired optokinetic nysta
Motor: Strength 5/5 in all major muscle groups without atrophy or fasiculations. Normal tone without cogwheeling. No abnormal or involuntary movements.
Reflexes: 2+ biceps, brachioradialis, and triceps bilaterally. 3+ patellar and ankle (without clonus) bilaterally. Positive snout and glabellar, but no palmomental or Hoffman's.
Sensation: Intact to light touch, pinprick, and temperature throughout. Vibration and proprioception intact at toes bilaterally. Romberg sign was absent.
Email comments: